Last Updated: August 22, 2023
Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
SKIN ULCERS
INDICATION – BRIEF
Skin ulcers are persistent open sores on the skin that fail to heal, typically on the lower legs, feet, or pressure points. Indications include ongoing sores lasting over two weeks, red, swollen, or painful sores, discoloration around the ulcer, and in severe cases, a foul odor. Clinical causes can be poor circulation, venous insufficiency, neuropathy, pressure, infections, autoimmune diseases, and malignancy. Non-clinical factors include smoking, poor nutrition, immobility, poor hygiene, and inadequate wound care. Early medical intervention is crucial to prevent worsening of the ulcer and avoid complications.
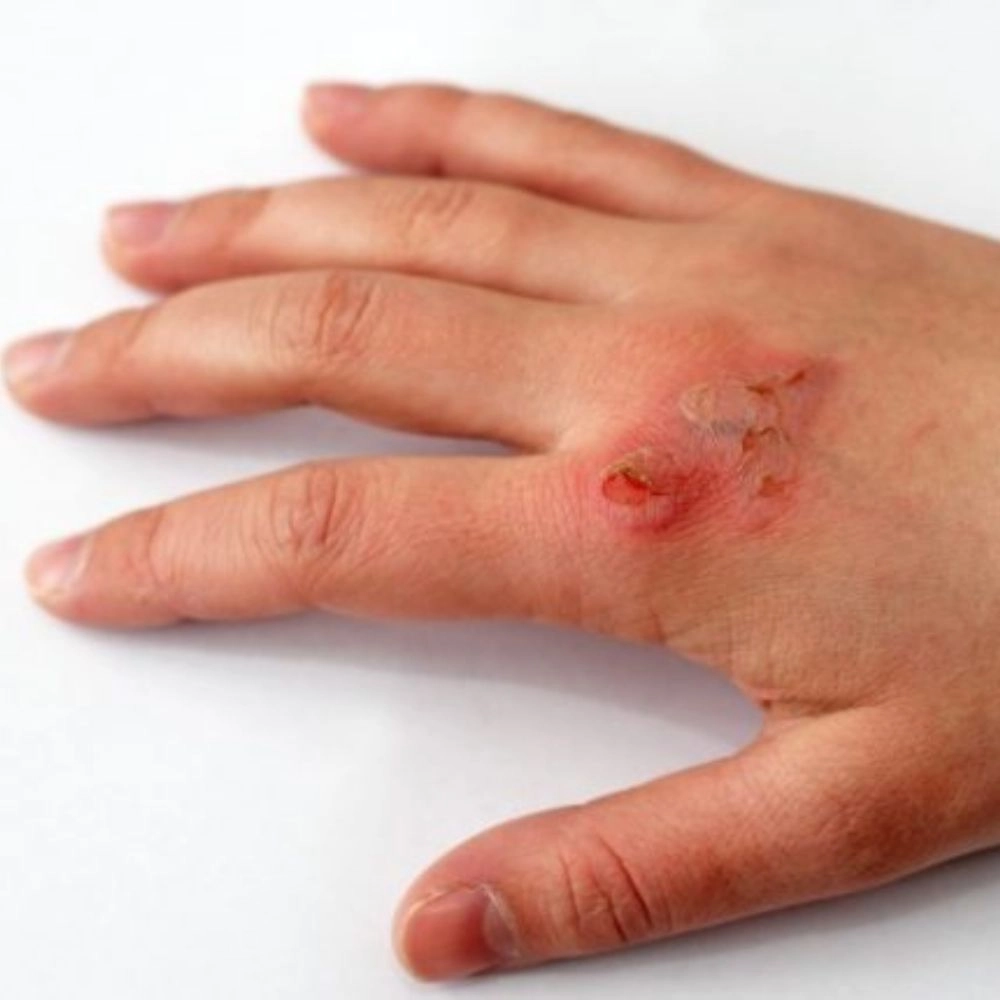
INDICATION – DEFINITION
Skin ulcers are open sores on the skin that don’t heal or keep returning. They usually develop on the lower legs, feet, or pressure points such as the buttocks. The indications of skin ulcers are as follows:
- Persistent open sore on the skin that lasts for more than two weeks.
- A red, swollen, painful sore or a sore that discharges pus.
- The skin around the ulcer may be discolored, often appearing darker or lighter.
- In severe cases, a foul odor may be present.
Now, there are a variety of factors that can cause skin ulcers, including:
Clinical Factors
- Poor Circulation: Conditions that result in poor blood circulation, like peripheral artery disease or diabetes, can lead to skin ulcers.
- Venous Insufficiency: This condition occurs when your leg veins don’t allow blood to flow back up to your heart, and it can cause venous skin ulcers.
- Neuropathy: Nerve damage, particularly in the legs and feet, can cause diabetic neuropathic ulcers.
- Pressure: Pressure ulcers, also known as bedsores, develop due to prolonged pressure on an area of skin, often affecting individuals who are bedridden or in a wheelchair.
- Infections: Certain infections, such as bacterial or viral infections, can lead to the development of skin ulcers.
- Autoimmune diseases: Conditions such as vasculitis, lupus, or scleroderma can cause ulcers on the skin.
- Malignancy: Certain types of skin cancers can present initially as non-healing ulcers.
Non-Clinical Factors
- Smoking: Smoking can impair blood circulation, thus contributing to the development of skin ulcers.
- Poor Nutrition: Malnutrition or deficiencies in certain vitamins and minerals can impair wound healing and increase the risk of skin ulcers.
- Immobility: Prolonged immobility can lead to pressure sores in susceptible individuals, especially those who are bedridden or use a wheelchair.
- Poor Hygiene: Poor skin hygiene may increase the risk of infection, which can lead to skin ulceration.
- Inadequate Wound Care: Insufficient or improper care of a wound can lead to the development of ulcers.
Remember, it’s crucial to seek medical attention if you notice any signs or symptoms of a skin ulcer.
SYMPTOMS AND DIAGNOSIS
Symptoms
Skin ulcers typically begin as a small sore, perhaps as a result of an injury where the skin breaks down and then they gradually get larger. Common symptoms include:
- A noticeable sore or wound, often on the lower legs or feet
- Pain or discomfort in the area of the ulcer
- Swelling, redness, or inflammation around the ulcer
- Discharge of pus or fluid from the ulcer
- Discoloration of the skin around the ulcer, often appearing darker or lighter
- In severe cases, the ulcer may have a foul odor
The skin around the ulcer might feel warm or hot, and the person could also have a fever, indicating an infection. If the ulcers are caused by poor circulation or diabetes, there may be numbness or a tingling sensation around the area.
Diagnosis
The diagnosis is usually based on the physical examination of the ulcer by a healthcare provider. They will assess the ulcer’s size, depth, and location, as well as any signs of infection.
Additional tests can help identify the underlying cause of the ulcer:
- Blood tests: Blood tests can check for conditions like diabetes or infection.
- Wound culture: This can determine if an infection is present and identify the type of bacteria causing it.
- Ankle-brachial index (ABI): This test compares blood pressure in your ankle with blood pressure in your arm to check for peripheral artery disease.
- Doppler ultrasound: This can evaluate blood flow in the veins and arteries of the legs.
- Biopsy: In some cases, a small sample of the ulcer may be taken for examination under a microscope to rule out malignancies or specific types of infections.
Remember, it’s essential to consult a healthcare provider if you notice symptoms of a skin ulcer. The earlier the diagnosis, the better the outcome is likely to be.
Prognosis and Impact

Prognosis
The prognosis for skin ulcers depends on several factors, including the cause, size, depth, location of the ulcer, the patient’s overall health, and the timeliness and effectiveness of treatment.
With appropriate treatment and management of underlying conditions, many skin ulcers can heal within weeks to months. However, some ulcers, particularly those associated with severe venous insufficiency or diabetes, can be challenging to treat and may become chronic, persisting for months to years, or may recur frequently.
In severe cases, especially when left untreated, skin ulcers can lead to serious complications such as cellulitis (skin infection), bone infection (osteomyelitis), gangrene, or even amputation in severe cases of diabetic foot ulcers.
Impact
Skin ulcers can significantly impact a person’s quality of life. Pain and discomfort associated with ulcers can affect mobility and daily activities. There’s also a psychological impact, as the presence of a chronic wound can lead to anxiety, depression, and social isolation.
From a socio-economic perspective, the treatment of skin ulcers can be costly, particularly for chronic or recurring ulcers. These costs include direct medical costs such as healthcare provider visits, medications, wound care supplies, and potential hospitalization, as well as indirect costs related to lost work productivity and caregiver time.
Management of skin ulcers thus not only focuses on healing the ulcer and treating the underlying cause but also on pain management, preventing complications, and improving the patient’s overall quality of life.
Treatment Options
- Wound Care: This is a crucial aspect of treatment. It involves cleaning the wound to prevent infection, applying dressings to keep the wound moist and promote healing, and debridement (removal of dead or infected tissue) when necessary.
- Compression Therapy: For venous ulcers, compression stockings or bandages are often used to help improve blood flow in the legs and reduce swelling.
- Topical or Oral Medications: Antibiotics may be needed if the ulcer is infected. Topical creams or gels can help promote wound healing or relieve pain. If the ulcer is caused by an autoimmune disease, medications to manage that condition may be used.
- Off-loading: For pressure ulcers and diabetic foot ulcers, off-loading (reducing pressure on the wound) is critical. This can involve the use of special footwear, wheelchairs, or mattresses.
- Vascular Procedures: If the ulcer is due to poor blood flow, procedures to improve circulation, such as angioplasty or bypass surgery, may be recommended.
- Hyperbaric Oxygen Therapy (HBOT): In some cases, particularly for hard-to-heal diabetic foot ulcers, HBOT may be used. This involves breathing pure oxygen in a pressurized chamber to promote healing.
- Skin grafts: In some cases, particularly if the ulcer is large or not healing well, a skin graft may be considered.
- Lifestyle changes: Managing underlying conditions (like diabetes), quitting smoking, improving nutrition, and exercising (if advised and safe to do) can aid in healing and preventing recurrence.
Each treatment plan is individualized based on the patient’s specific needs and underlying health. It’s crucial to closely follow the healthcare provider’s instructions to ensure the best possible healing outcomes. Ongoing follow-up care is also important to monitor the healing process and make necessary adjustments to the treatment plan.
Risks and Side Effects
- Wound Care: Side effects can include pain during cleaning or debridement procedures. There’s also a risk of potential allergic reactions to certain topical medications or dressings.
- Compression Therapy: These can sometimes be uncomfortable and cause skin irritation. If not used correctly, they could potentially impair circulation.
- Topical or Oral Medications: Topical treatments can cause skin irritation, redness, or rash. Oral antibiotics can lead to side effects like nausea, diarrhea, or allergic reactions. Long-term use of antibiotics may lead to antibiotic resistance.
- Off-loading: The devices used for off-loading can sometimes be uncomfortable or awkward to use, and there’s a risk of skin irritation or injury if not used correctly.
- Vascular Procedures: As with any surgical procedure, these carry risks such as infection, bleeding, blood clots, and reactions to anesthesia. There’s also the risk that the procedure may not improve circulation as expected.
- Hyperbaric Oxygen Therapy (HBOT): Potential side effects include ear or sinus pain, fatigue, anxiety from being in a confined space (claustrophobia), temporary short-sightedness (myopia), and risk of lung collapse or oxygen poisoning if the pressure changes are too rapid.
- Skin grafts: Risks include infection, bleeding, graft failure, and scarring. There could also be pain or complications at the donor site (the area of skin where the graft was taken from).
- Lifestyle changes: Generally, these carry minimal risks. However, individuals should consult with their healthcare provider before starting a new exercise regimen, especially if they have chronic health conditions.
FAQ Section
Skin ulcers are open sores that do not heal or keep returning. They can occur anywhere on the body but are more common on the lower legs, feet, and pressure points such as the buttocks.
Symptoms of a skin ulcer include a noticeable sore or wound, often on the lower legs or feet, pain or discomfort in the area, swelling, redness, or inflammation around the ulcer, and discharge of pus or fluid. In severe cases, the ulcer may have a foul odor.
Skin ulcers can be caused by a range of factors, including poor circulation, venous insufficiency, neuropathy, pressure, infections, autoimmune diseases, malignancy, smoking, poor nutrition, immobility, poor hygiene, and inadequate wound care.
Skin ulcers are typically diagnosed through a physical examination by a healthcare provider. Additional tests like blood tests, wound culture, Ankle-brachial index, Doppler ultrasound, or biopsy may be used to determine the underlying cause.
Treatment options for skin ulcers include wound care, compression therapy, medications, off-loading, vascular procedures, hyperbaric oxygen therapy, skin grafts, and lifestyle changes.
Side effects can vary depending on the specific treatment, but may include pain, skin irritation, redness, rash, discomfort, nausea, diarrhea, risks associated with surgical procedures, and potential complications from medications or therapies.
While not all skin ulcers can be prevented, managing underlying conditions, maintaining good hygiene, ensuring adequate nutrition, avoiding prolonged pressure on the skin, and seeking early treatment for wounds can help reduce the risk.
The prognosis depends on many factors, including the cause, size, depth, location of the ulcer, the patient’s overall health, and the effectiveness of treatment. With appropriate treatment, many ulcers can heal within weeks to months, but some may become chronic or recur frequently.
Skin ulcers can significantly impact a person’s quality of life due to pain, discomfort, mobility issues, and psychological effects such as anxiety and depression. There can also be economic implications related to treatment costs and lost work productivity.
