Last Updated: August 22, 2023
Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
SKIN FUNGAL INFECTION
INDICATION – BRIEF
Skin fungal infections, caused by various fungi, occur when these organisms overgrow on skin, hair, or nails. They are more common in people with weakened immune systems, peripheral vascular disease, or pre-existing skin conditions. Non-clinical factors include poor hygiene, excess moisture, shared surfaces (like in gyms or pools), warm and humid climate, tight clothing, and certain jobs with frequent water exposure or occlusive footwear. Common types include athlete’s foot, jock itch, ringworm, and yeast infections. Treatments involve antifungal creams or oral medication, and preventive measures include maintaining hygiene, keeping skin dry, and wearing breathable clothing. A healthcare provider should be consulted for symptoms.
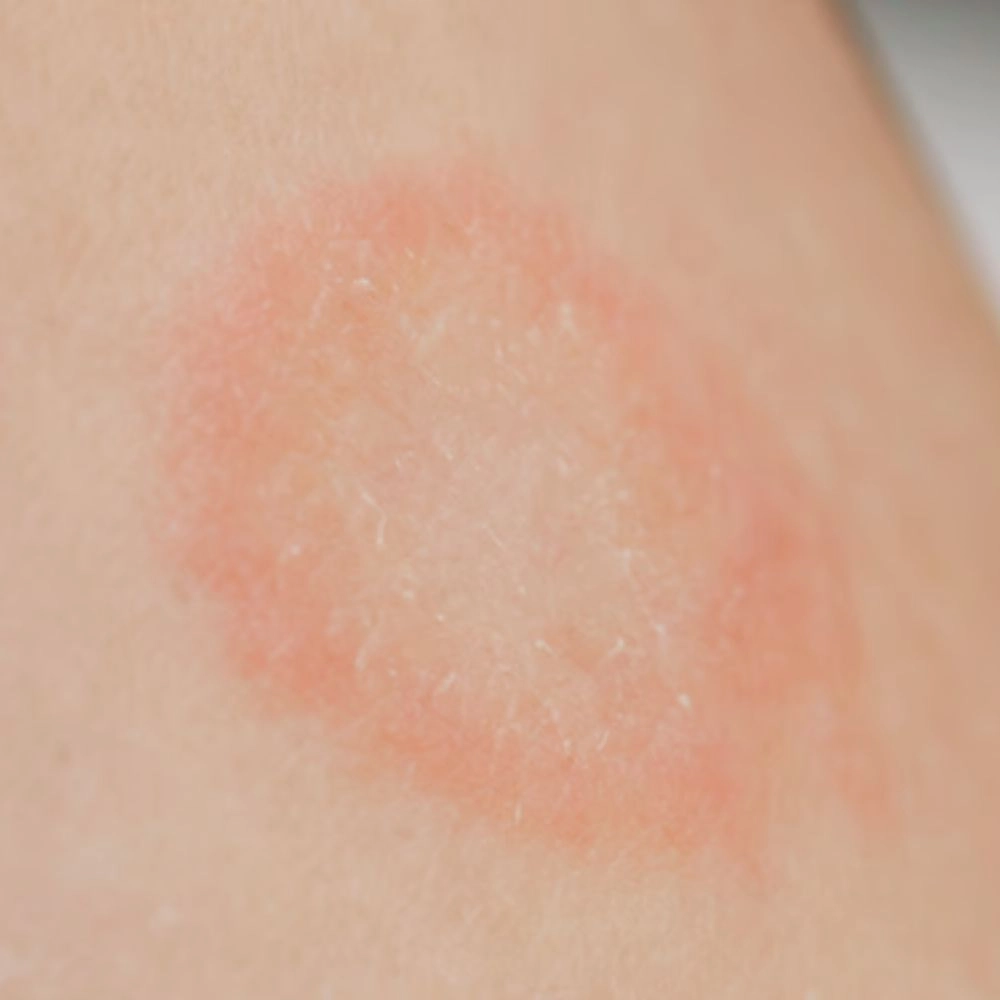
INDICATION – DEFINITION
Indication: Skin Fungal Infections
Skin fungal infections are caused by various types of fungi, including dermatophytes and yeasts. These fungi can live on the dead tissues of the hair, nails, and outer skin layers.
Clinical Causal Factors
- Immune System: People with weakened immune systems, like those with HIV/AIDS, diabetes, or undergoing treatments such as chemotherapy, are at higher risk of fungal infections as their body might not be able to control the growth of fungi effectively.
- Peripheral Vascular Disease: Poor blood circulation, particularly in the extremities, may lead to conditions conducive to fungal growth, such as excess moisture or skin maceration.
- Pre-existing Skin Conditions: Conditions like psoriasis or eczema that compromise the skin barrier can predispose individuals to fungal infections.
Non-Clinical Causal Factors
- Hygiene and Moisture: Fungi love warm, moist environments. Poor hygiene or staying in sweaty clothes can create such an environment, particularly in skin folds and between the toes.
- Shared Surfaces: Fungi can survive on surfaces and can spread in shared areas like gyms, swimming pools, or by sharing towels or shoes.
- Climate: Living in a warm, humid climate can also predispose an individual to fungal infections.
- Clothing: Tight, non-breathable clothing can trap moisture and heat, creating an ideal environment for fungi.
- Occupational Exposure: Jobs that involve frequent water exposure or wearing occlusive footwear (like rubber boots) may increase the risk of fungal infections.
Common types of skin fungal infections include athlete’s foot, jock itch, ringworm, and yeast infections. Treatment often involves antifungal creams, ointments, or, in more severe cases, oral medication. Maintaining good hygiene, keeping the skin dry and clean, avoiding shared surfaces, and wearing breathable clothing can help prevent fungal infections.
However, please note that this advice is general in nature. If you or someone else has symptoms of a fungal infection, you should consult with a healthcare provider for a proper diagnosis and treatment plan.
SYMPTOMS AND DIAGNOSIS
Symptoms
Symptoms of skin fungal infections can vary depending on the type of fungus involved and the body part affected, but they commonly include:
- Redness and Itching: This is typically the first symptom. The affected area often becomes red and itchy.
- Scaling, Cracking, and Peeling Skin: The skin may become scaly, crack, or start to peel.
- Rashes or Patches: There might be visible rashes, and sometimes patches that may be redder around the outside with normal skin tone in the center. This may create the appearance of a ring, hence the term “ringworm.”
- Changes in Nail Appearance: If nails are infected, they can become discolored, thickened, brittle, and may even separate from the nail bed.
- Blisters and Pustules: In some cases, blisters and pustules might form, often filled with pus.
Diagnosis
A dermatologist or other healthcare provider usually diagnoses skin fungal infections by:
- Physical Examination: They will begin with a physical examination of the affected area.
- Microscopic Examination: A scraping of skin, nail clippings, or some hairs may be taken and examined under a microscope to identify the type of fungus.
- Culture: In some cases, the sample may be sent to a lab to be cultured and identify the specific type of fungus causing the infection.
- Wood’s Lamp Examination: A special type of light, called a Wood’s lamp, may be used to illuminate the area and see if the infection will fluoresce.
- Biopsy: In rare instances, a skin biopsy might be required if the diagnosis is unclear or the infection is not responding to treatment.
It’s important to remember that while these are common symptoms and diagnostic methods for skin fungal infections, only a healthcare provider can make a definitive diagnosis and recommend appropriate treatment.
Prognosis and Impact

Prognosis
The prognosis for skin fungal infections is generally good, but it depends on various factors like the specific type of fungus, the location and size of the infection, the person’s overall health, and how promptly they receive treatment.
- Resolution with Treatment: Most fungal infections resolve completely with appropriate treatment, which can include topical antifungal creams or, in more serious cases, oral antifungal medications.
- Recurrence: Some fungal infections, particularly those affecting the nails and feet (like athlete’s foot), have a tendency to recur, especially if preventative measures aren’t followed.
- Complications: If left untreated, or in individuals with compromised immune systems, skin fungal infections may spread to other parts of the body or lead to secondary bacterial infections.
Impact
- Physical Discomfort: The main impact of skin fungal infections is physical discomfort. This can include itching, burning, and pain, especially if the infection is widespread or located in sensitive areas.
- Psychological Impact: The appearance of skin fungal infections can lead to self-consciousness and stress, potentially affecting a person’s self-esteem and quality of life.
- Lifestyle Changes: Managing a persistent or recurrent fungal infection may require changes to a person’s routine, including more diligent hygiene practices, changes in clothing choices, or avoidance of certain activities (like swimming).
- Healthcare Costs: Recurring or persistent fungal infections can lead to increased healthcare costs, from both treatments and the need for ongoing medical consultations.
Treatment Options
- Topical Antifungals: These are usually the first line of treatment for skin fungal infections. They are applied directly to the skin, nail, or scalp, and come as creams, lotions, powders, gels, or shampoos. Examples include clotrimazole (Lotrimin), miconazole (Micatin), terbinafine (Lamisil), and ketoconazole (Nizoral).
- Oral Antifungals: For more severe infections, oral antifungal medications may be prescribed. These include drugs like fluconazole (Diflucan), itraconazole (Sporanox), and terbinafine (Lamisil).
- Medicated Nail Creams or Lacquers: For fungal nail infections, a doctor might prescribe an antifungal nail cream or a nail lacquer like ciclopirox (Penlac).
- Nail Removal: In severe or resistant cases of nail fungal infections, the nail may need to be removed surgically or with a strong acidic solution to allow a new, healthier nail to grow in.
In addition to medication, lifestyle modifications are crucial. Keeping the skin clean and dry, avoiding shared surfaces in public spaces, and not sharing personal items can help prevent and treat skin fungal infections.
Risks and Side Effects
- Topical Antifungals: These are generally well-tolerated. However, some people may experience skin irritation, redness, burning, itching, or stinging at the application site. Allergic reactions are rare but can occur.
- Oral Antifungals: These can cause more significant side effects as they affect the entire body. Potential side effects include gastrointestinal issues (like nausea, vomiting, diarrhea), headache, rash, and changes in taste. In rare cases, they can cause liver damage, so your doctor may monitor your liver function during treatment. As these medications can interact with other drugs, it’s important to tell your healthcare provider about all the medications you’re taking.
- Medicated Nail Creams or Lacquers: These can sometimes cause skin irritation around the treated nail. There might be changes in the nail’s shape, color, or texture.
- Nail Removal: This procedure can cause pain, and there’s a risk of infection or reaction to the anesthetic. After the procedure, the nail may grow back misshapen or discolored.
Also, improper or incomplete treatment can lead to a risk of the infection recurring or spreading to other parts of the body. Fungal infections can be stubborn, and even after successful treatment, there’s a possibility that they may return, particularly if preventative measures are not strictly followed.
FAQ Section
Skin fungal infections are caused by various types of fungi, including dermatophytes and yeasts. These fungi can overgrow on the skin due to factors like a weakened immune system, pre-existing skin conditions, poor hygiene, a warm and humid climate, and frequent exposure to shared surfaces like gyms or pools.
Symptoms can vary depending on the type of fungus and the location of the infection, but commonly include redness, itching, scaling or peeling skin, changes in nail appearance if nails are affected, and sometimes blisters or pustules. If you notice these symptoms, you should consult with a healthcare provider.
Diagnosis typically involves a physical examination, microscopic examination of a skin, nail, or hair sample, and occasionally a culture or biopsy. In some cases, a Wood’s lamp examination may be used.
Treatment usually involves antifungal medications, which can be topical (applied to the skin) or oral. For nail infections, medicated nail creams or even nail removal may be necessary. Lifestyle modifications, such as improved hygiene and avoidance of shared surfaces, are also important.
Side effects depend on the type of treatment. Topical antifungals can cause skin irritation, while oral antifungals can cause gastrointestinal issues and in rare cases, liver damage. Medicated nail creams may cause skin irritation around the nail, and nail removal can cause pain and risk of infection.
Yes, maintaining good skin hygiene, wearing breathable clothing, keeping your skin dry, and avoiding shared surfaces can help prevent fungal infections.
Yes, some types of fungal infections, especially those affecting nails and feet, can recur. Following the full course of treatment and maintaining preventative measures can reduce the risk of recurrence.
While generally not life-threatening, skin fungal infections can cause discomfort due to itching or pain and can impact one’s self-esteem due to their appearance. They may require lifestyle changes and can lead to increased healthcare costs if recurrent or persistent.
If you think you have a skin fungal infection, consult a healthcare provider for a proper diagnosis and treatment plan. Do not attempt to self-diagnose or treat a suspected fungal infection without medical advice.
