Last Updated: August 22, 2023
Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
PSORIASIS
INDICATION – BRIEF
Psoriasis is a chronic autoimmune skin disorder characterized by red, itchy, and scaly patches. Its exact cause is unknown, but it involves a malfunction of the immune system and often has a genetic component. Clinical factors include genetics and an overactive immune system. Non-clinical factors encompass stress, infections, alcohol and tobacco use, certain medications, and skin injury. These factors can trigger the disease or exacerbate its symptoms. Each individual’s experience with psoriasis varies greatly, making consultation with a healthcare provider crucial for a comprehensive evaluation and tailored treatment plan, which can include medical treatments and lifestyle modifications.
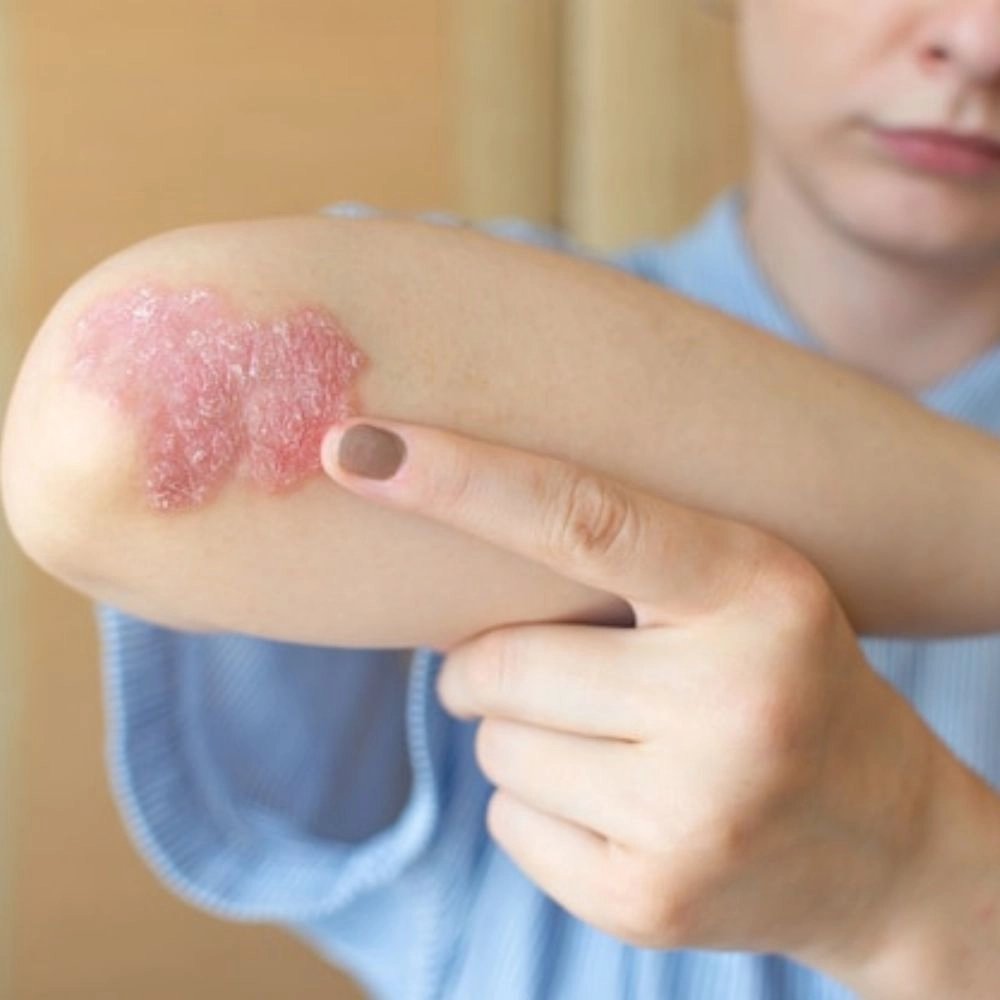
INDICATION – DEFINITION
Psoriasis: Psoriasis is a chronic autoimmune skin disease that accelerates the skin cell life cycle. It results in patches of skin that are typically red, itchy, and scaly. The patches can vary in size from small, localized areas to complete coverage of the body. It’s non-contagious and can occur at any age, though it most commonly presents between the ages of 15 and 35.
Causal factors: The exact cause of psoriasis is unknown, but it is thought to be related to an immune system problem with T cells and other white blood cells, called neutrophils, in your body.
Clinical factors
- Genetics: Psoriasis can run in families, indicating a genetic predisposition. If one or both parents have psoriasis, their children are more likely to develop the condition.
- Immune system: In psoriasis, the immune system attacks healthy skin cells by mistake, causing the rapid buildup of skin cells and forming scaly patches.
Non-Clinical factors
- Stress: High stress levels can cause psoriasis flare-ups and also make treatment less effective.
- Infections: Certain infections, like strep throat or skin infections, can trigger the onset of psoriasis or exacerbate existing psoriasis.
- Alcohol and Tobacco: Excessive alcohol consumption and tobacco smoking can both increase the risk of developing psoriasis and exacerbate existing conditions.
- Medications: Certain medications, such as lithium, antimalarial drugs, and high blood pressure medications, may worsen psoriasis or trigger it.
- Injury to the skin: This includes cuts, burns, and insect bites. This is known as the Koebner phenomenon.
Please remember that psoriasis can be a complex condition, and its onset and progression can vary greatly between individuals. It’s essential for patients to consult with a dermatologist or healthcare provider for a comprehensive evaluation and treatment plan.
Managing psoriasis often involves a combination of medical treatments and lifestyle modifications to mitigate triggers. Treatments can range from topical creams to light therapy and systemic medications, depending on the severity of the condition.
SYMPTOMS AND DIAGNOSIS
Symptoms
The symptoms can vary from person to person, but common signs typically include:
- Red patches of skin covered with thick, silvery scales
- Small, scaly spots (commonly seen in children)
- Dry, cracked skin that may bleed or itch
- Itching, burning, or soreness around patches
- Thickened, pitted, or ridged nails
- Swollen and stiff joints
Psoriasis patches can range from a few spots of dandruff-like scaling to major eruptions that cover large areas. Most types of psoriasis go through cycles, flaring for a few weeks or months, then subsiding for a time or even going into complete remission.
Diagnosis
There is no definitive test for psoriasis. A dermatologist usually makes a diagnosis based on the appearance of the skin and symptoms described by the patient. Steps for diagnosing psoriasis typically include:
- Physical Examination: Your dermatologist will carefully examine your skin, scalp, and nails.
- Medical History: The dermatologist will ask about your health history, including if any family members have psoriasis.
- Skin Biopsy: In some cases, your dermatologist may take a small sample of skin (biopsy). They will examine this under a microscope to confirm the diagnosis and to rule out other similar conditions.
The severity of psoriasis is determined by how much of your body surface area (BSA) is affected. Psoriasis is considered mild if less than 3% of the BSA is affected, moderate if 3-10% of the BSA is affected, and severe if more than 10% of the BSA is affected.
Prognosis and Impact

Prognosis
Psoriasis is a chronic condition, meaning it’s long-lasting. There is currently no cure for psoriasis, but with the right treatment, it can be managed effectively in most people. Some may experience periods of complete remission, where they have no symptoms at all. However, flare-ups, where the condition worsens for a period, are common.
The effectiveness of treatments can also vary greatly between individuals. Some people may find that certain treatments become less effective over time, and it may be necessary to switch to a different treatment.
Impact
Psoriasis can have a significant impact on quality of life. The physical discomfort caused by the symptoms – itching, pain, and skin cracking – can be quite considerable.
In addition to physical effects, psoriasis can also have emotional and social impacts. The visible nature of the skin lesions can lead to embarrassment, self-consciousness, or social withdrawal. There’s also a higher incidence of depression and anxiety among people with psoriasis.
Furthermore, psoriasis has been associated with a number of other health conditions. These include psoriatic arthritis, a type of joint disease, as well as increased risk for cardiovascular disease, metabolic syndrome, and other autoimmune diseases.
In conclusion, the prognosis of psoriasis can be varied and its impact is significant, affecting both the physical and mental health of those who live with the condition. But with the right treatment and management strategies, most people with psoriasis can lead fulfilling, active lives.
Treatment Options
Topical treatments: These are usually the first-line therapy for mild to moderate psoriasis and are applied directly to the skin. They include corticosteroids, vitamin D analogues, retinoids, calcineurin inhibitors, coal tar, and salicylic acid.
Phototherapy (Light therapy): This involves exposing the skin to ultraviolet (UV) light under medical supervision. Types of phototherapy include UVB phototherapy, psoralen plus ultraviolet A (PUVA), and excimer laser.
Systemic medications: These are prescription drugs that are taken orally or by injection and work throughout the body. They are typically used for individuals with moderate to severe psoriasis and/or psoriatic arthritis. These medications include methotrexate, cyclosporine, biologics (such as etanercept, infliximab, adalimumab, ustekinumab, and others), and new oral treatments like apremilast.
Lifestyle and home remedies: These involve daily routines and habits that can help manage the condition. Regular moisturizing, quitting smoking and alcohol, maintaining a healthy weight, and managing stress can all improve psoriasis.
Please consult with your healthcare provider or a dermatologist to discuss the most suitable treatment options for your situation
Risks and Side Effects
Topical treatments:
- Corticosteroids: Long-term use or overuse can lead to skin thinning, irritation, dryness, acne, and changes in skin color.
- Vitamin D analogues: These can cause skin irritation or sensitivity.
- Retinoids: They can cause skin irritation and increased sensitivity to sunlight.
- Calcineurin inhibitors: Long-term use can increase the risk of skin infections and lymphoma.
- Coal tar: It can cause skin irritation, staining of clothing and bedding, and increased sensitivity to sunlight.
- Salicylic acid: Overuse can lead to skin irritation and weakness.
Phototherapy (Light therapy):
- UVB phototherapy: Can cause skin dryness and irritation, increased risk of skin cancer, and increased sensitivity to sunlight.
- Psoralen plus ultraviolet A (PUVA): Can lead to nausea, headache, burning, itching, increased risk of skin cancer, and cataracts if eye protection isn’t used.
- Excimer laser: May result in blistering and changes in skin color.
Systemic medications:
- Methotrexate: Side effects can include liver damage, lung damage, decreased white blood cell count leading to increased susceptibility to infections, and potential birth defects if taken during pregnancy.
- Cyclosporine: Can cause kidney problems, high blood pressure, and increased susceptibility to infections.
- Biologics: Can increase the risk of infections, cause injection site reactions, and in rare cases, trigger other autoimmune disorders.
- Apremilast: May cause diarrhea, nausea, headache, respiratory infections, and depression.
Lifestyle and home remedies: Most lifestyle changes have few risks but consult with a healthcare provider if you are unsure.
While some of these side effects can sound alarming, remember that these treatments are usually only prescribed if the potential benefits outweigh the risks. Side effects can often be managed and may go away over time. Regular monitoring by a healthcare professional can ensure that any adverse effects are detected and managed promptly.
FAQ Section
Psoriasis is a chronic autoimmune skin disorder that causes red, itchy, and scaly patches. It occurs when the immune system mistakenly accelerates the life cycle of skin cells.
No, psoriasis is not contagious. You cannot catch it from touching someone who has it, nor can you pass it onto others.
Several factors can trigger psoriasis, including stress, infections, certain medications, alcohol and tobacco use, and skin injuries. However, triggers can vary greatly from person to person.
Currently, there is no cure for psoriasis. However, there are various treatments available that can help manage the symptoms and even achieve periods of remission.
A: Yes, psoriasis is associated with several other health conditions, including psoriatic arthritis, cardiovascular disease, and other autoimmune diseases. It can also have significant psychological impacts.
Treatment options include topical treatments (applied to the skin), phototherapy (light therapy), systemic medications (oral or injectable drugs), and lifestyle changes. The choice of treatment depends on the severity of the condition and the patient’s overall health.
All treatments can potentially cause side effects. These can range from skin irritation with topical treatments to increased risk of infections with systemic medications. It’s important to discuss these with your healthcare provider before starting any new treatment.
Psoriasis can significantly affect quality of life. The physical discomfort and visible skin lesions can lead to emotional distress and social isolation. It’s important to seek support and effective treatments to manage the condition.
Absolutely, lifestyle changes such as regular moisturizing, quitting smoking and alcohol, maintaining a healthy weight, and managing stress can all improve psoriasis symptoms.
While both can cause red, itchy skin, they are distinct conditions. Psoriasis typically causes thick, silvery scales with well-defined edges, while eczema tends to cause itchy, inflamed, and sometimes blistering skin. A healthcare provider can provide an accurate diagnosis.
