Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
PSEUDOFOLLICULITIS
INDICATION – BRIEF
Pseudofolliculitis barbae, or razor bumps, is a common condition in individuals with tightly curved or kinky hair, particularly African American, Hispanic, and South Asian men. It occurs when the hair curls back into the skin, causing inflammation and scarring. Factors like close shaving, genetics, hair care practices, occupational demands, and skincare routines contribute to its development. Management involves allowing the beard to grow for a few weeks, using single-blade or electric clippers for shaving, and maintaining proper skincare. Topical antibiotics, retinoids, and chemical peels may be used. The 1064 nm Nd:YAG laser is effective for hair removal. Overall, pseudofolliculitis barbae requires a combination of hair care, shaving techniques, and skincare to minimize its impact.
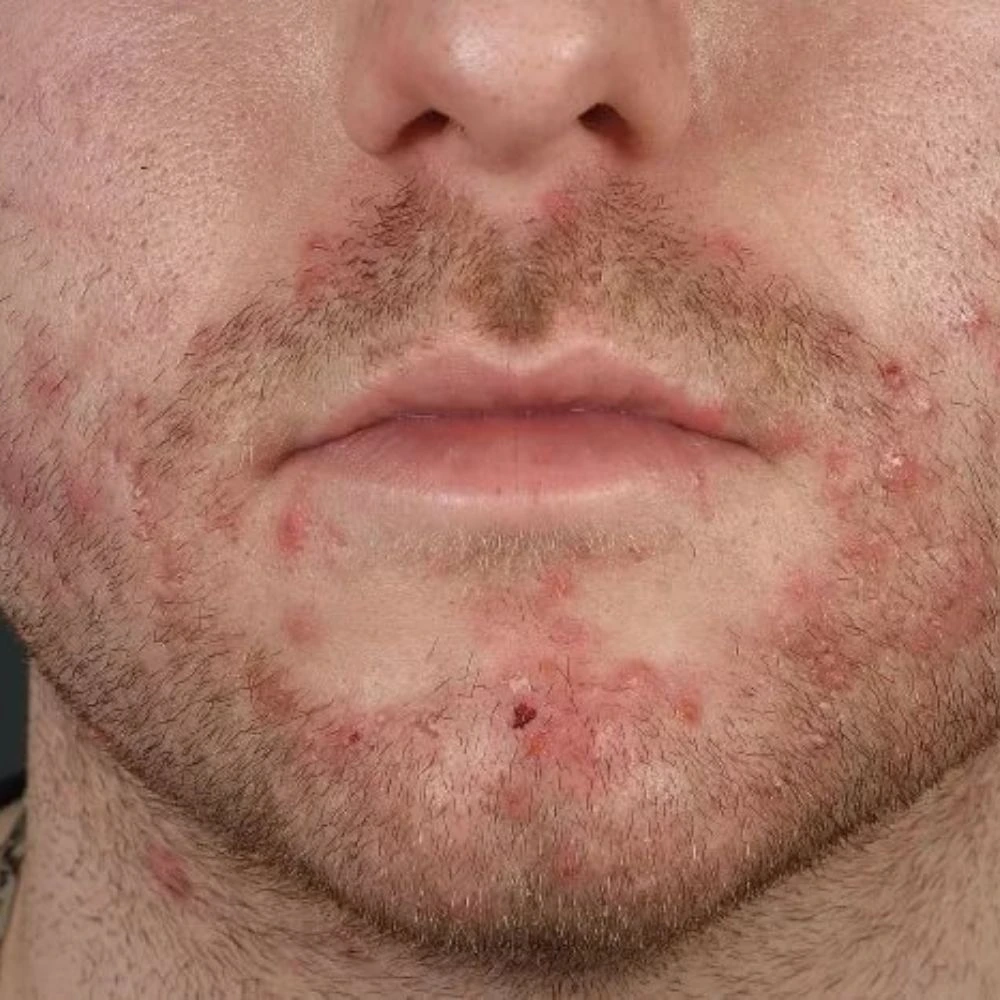
INDICATION – DEFINITION
Pseudofolliculitis barbae, commonly referred to as “razor bumps,” is a common condition of the beard area occurring in up to 60% of African American men and other people with curly hair. It is also known to affect certain Hispanic populations and South Asian men. The problem results when highly curved hairs grow back into the skin causing inflammation and a foreign body reaction. Over time, this can cause keloidal scarring which looks like hard bumps of the beard area and neck.
Clinical factors
- Hair type: The main factor that predisposes an individual to pseudofolliculitis barbae is having tightly curved or kinky hair. This type of hair tends to curl back into the skin instead of growing straight out of the follicle.
- Shaving techniques: Close shaving typically exacerbates the condition as it allows the tip of the hair to retreat below the skin surface. When it starts to grow again, it can pierce the follicular wall and incite an inflammatory response.
- Genetic factors: Certain individuals are genetically predisposed to develop this condition, often due to the characteristics of their hair and follicles.
Non-Clinical factors
- Hair care practices: The frequency and method of shaving can greatly influence the development of pseudofolliculitis barbae. Using a single-blade razor or electric shaver can help reduce the occurrence of razor bumps, as can shaving in the direction of hair growth.
- Occupational demands: Some jobs require a clean-shaven face, which increases the frequency of shaving and the risk of developing pseudofolliculitis barbae.
- Skin care routines: Lack of proper skincare routine and inappropriate skincare products can worsen the condition. It’s important to keep the skin clean and moisturized, and to exfoliate periodically to remove dead cells and help keep the follicles open.
Management involves letting the beard grow for 3–4 weeks to remove the offending hair. Shaving should be done with a single blade or wire-wrapped blade. Electric clippers are also useful. Topical or oral antibiotics may be required during flare-ups and maintenance therapy includes topical retinoids, salicylic acid, and glycolic acid peels. The 1064 nm Nd:YAG laser offers the best results for hair removal for this condition.
SYMPTOMS AND DIAGNOSIS
Pseudofolliculitis barbae, or razor bumps, is a skin condition that typically affects individuals with curly or coarse hair who shave regularly. Here are some of the most common symptoms and how the diagnosis is made:
Symptoms
- Razor Bumps: The primary symptom of pseudofolliculitis barbae is the presence of small, inflamed bumps or pimples on the shaved area, commonly the face and neck. These bumps can be itchy, painful, and may become filled with pus.
- Hyperpigmentation: With time, the affected skin can darken, a condition known as post-inflammatory hyperpigmentation.
- Ingrown Hairs: Since the hair grows back into the skin, it can sometimes be seen as a small, dark hair loop within the bumps.
- Scarring: If left untreated, pseudofolliculitis barbae can lead to scarring, including the formation of keloids, particularly in people with darker skin tones.
Diagnosis
The diagnosis of pseudofolliculitis barbae is usually made based on the patient’s symptoms and a physical examination of the affected skin. A dermatologist will look for the characteristic appearance of small, inflamed bumps in the beard area, often with associated dark spots and evidence of ingrown hairs.
Your dermatologist might take a close-up photograph of the skin or use a dermoscope — a handheld microscope — to examine the skin in detail. In some cases, a skin biopsy might be performed if the diagnosis is unclear or if other skin conditions need to be ruled out.
Once the condition is diagnosed, the dermatologist can then recommend the most appropriate treatment options. These might include modifications to shaving practices, use of specific skincare products, prescription medications, or possibly laser hair removal.
Prognosis and Impact

Prognosis
Pseudofolliculitis barbae (PFB) is a chronic condition that can be managed effectively but may not be entirely curable, mainly because it’s often related to hair growth patterns and personal or occupational shaving requirements.
If patients can avoid close shaving, the prognosis is generally excellent, and the condition can often resolve without further intervention. However, in individuals who must shave regularly, the condition can recur.
Medications such as topical retinoids and antibiotics, as well as appropriate hair removal methods, can reduce the frequency and severity of outbreaks. Procedures like laser hair removal can offer a more long-term solution, but the response to treatment can vary between individuals.
Impact
The impact of PFB can extend beyond physical symptoms, especially given its location on the face and neck. The condition can significantly affect an individual’s self-esteem and social interactions due to the visible and sometimes distressing appearance of the lesions.
The chronic nature of PFB can also lead to frustration and distress, as the condition may require ongoing management and changes in personal care routines. It can lead to avoidance of social activities and cause significant emotional distress.
From a physical standpoint, untreated or poorly managed PFB can lead to post-inflammatory hyperpigmentation (dark spots), keloidal or hypertrophic scarring, and potentially secondary bacterial infection.
In occupational settings where a clean shave is required (like military or certain corporate settings), this condition can interfere with job duties and lead to significant professional issues.
Therefore, effective management of PFB is critical, not just to alleviate physical symptoms but also to minimize the potential psychological and social impact of the condition.
Treatment Options
The treatment of pseudofolliculitis barbae is usually directed at achieving two main goals: easing any present symptoms and preventing new ones from developing. Here are some of the commonly used treatment options:
Behavioral Modification:
- Shaving Techniques: Altering the way you shave is one of the first steps in treating this condition. Patients are advised to avoid close shaves, shave in the direction of hair growth, use a single blade or special wire-wrapped blade to avoid close shaves, and not to stretch the skin while shaving.
- Alternative Hair Removal Methods: Use of electric clippers set at a level that leaves short stubble can be beneficial. Alternatively, depilatory creams that chemically cut the hair at the surface of the skin can be useful but can also cause skin irritation in some individuals.
Medications:
- Topical Retinoids: Creams like tretinoin can help by exfoliating the skin and reducing the amount of ingrown hairs.
- Topical Antibiotics: These can help reduce inflammation and control secondary infections.
- Topical Corticosteroids: These can be used to reduce inflammation associated with PFB.
- Topical Eflornithine: This cream slows facial hair growth in women and can also be helpful in men.
Procedures:
- Laser Hair Removal: This method can result in long-term reduction of hair growth, and as a result, decrease the occurrence of PFB. It’s most effective in individuals with dark hair and light skin, although newer lasers can be effective in individuals with darker skin tones as well.
- Chemical Peels: Salicylic acid and glycolic acid peels can help exfoliate the skin, open up clogged pores, and reduce the occurrence of ingrown hairs.
Treatment plans should be individualized to the patient’s specific needs, including their tolerance to certain treatments, skin type, and the severity of their condition.
Risks and Side Effects
Behavioral Modification:
- Shaving Techniques: Changing the way one shaves might not result in immediate improvements and might take some getting used to. Incorrect techniques might lead to cuts or scrapes.
- Alternative Hair Removal Methods: Depilatory creams can sometimes cause skin irritation, burns, or allergic reactions. Using electric clippers improperly can lead to cuts and potential infections.
Medications:
- Topical Retinoids: These can cause skin irritation, redness, dryness, and sensitivity to the sun. They are also teratogenic, meaning they can cause birth defects, so they are not recommended for use during pregnancy.
- Topical Antibiotics: Prolonged use can lead to antibiotic resistance. They can also cause skin irritation or allergic reactions.
- Topical Corticosteroids: Long-term use can cause thinning of the skin, redness, acne, and stretch marks.
- Topical Eflornithine: Side effects include stinging, burning, redness, and skin rash. It’s also not recommended for use in individuals under the age of 18.
Procedures:
- Laser Hair Removal: Possible side effects include pain during treatment, skin irritation, pigment changes (either lightening or darkening of the skin), and, rarely, blistering or scarring. It can also be a relatively costly treatment option.
- Chemical Peels: Potential side effects include redness, irritation, and peeling. There’s also a risk of discoloration, particularly in individuals with darker skin tones.
While there are potential risks and side effects with each treatment option, your dermatologist will work with you to find the most appropriate and effective treatment while minimizing any adverse effects.
FAQ Section
Pseudofolliculitis barbae, often referred to as ‘razor bumps,’ is a common skin condition that occurs when hair curls back into the skin, leading to inflammation. It typically affects people with curly or coarse hair, particularly in the beard area.
This condition is primarily caused by shaving, especially close shaving. The sharp, cut hair can curl back into the skin, leading to inflammation and the formation of razor bumps. Factors such as having tightly curved or coarse hair, poor shaving techniques, and frequent shaving can increase the risk.
Some effective preventive measures include improving shaving techniques, like not shaving too closely, using a single-blade razor, and shaving in the direction of hair growth. Using electric clippers or depilatory creams can also be helpful. In addition, keep your skin clean and moisturized to maintain overall skin health.
While there is no definitive cure for pseudofolliculitis barbae, the condition can be effectively managed. Treatment involves a combination of changes in hair removal practices and possibly medications to reduce inflammation and prevent infection. In some cases, procedures like laser hair removal or chemical peels may be recommended.
Yes, treatments for pseudofolliculitis barbae can have side effects. For instance, topical retinoids can cause skin dryness and irritation, while laser hair removal can cause skin pigment changes. It’s important to discuss these potential side effects with your dermatologist before starting any new treatment.
The condition can affect individuals both physically and psychologically. Physically, it may cause discomfort, itching, and potentially lead to scarring if left untreated. Psychologically, the visible nature of the condition can affect self-esteem and social interactions.
Yes, women can also get pseudofolliculitis barbae, especially if they have coarse or curly hair and shave regularly. However, it’s more common in areas like the underarms or legs rather than the facial area.
If left untreated, pseudofolliculitis barbae can lead to complications such as bacterial infections, dark spots (hyperpigmentation), and scarring, including keloidal scars. Therefore, it’s important to consult a dermatologist if you have symptoms of this condition.
