Last Updated: August 22, 2023
Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
NEVUS
INDICATION – BRIEF
A nevus, or mole, is a skin growth that arises due to the proliferation of melanocytes, the pigment-producing cells in the skin. They can be influenced by several clinical factors like genetics, immune status, and hormonal changes. Non-clinical factors include sun exposure, age, and skin type, with individuals having lighter skin, hair, eyes, or those who sunburn easily being more prone to developing nevi. Most nevi are benign, but some can evolve into melanoma, a severe type of skin cancer. Regular skin checks are crucial to detect any changes in a mole’s characteristics, indicating potential malignancy.
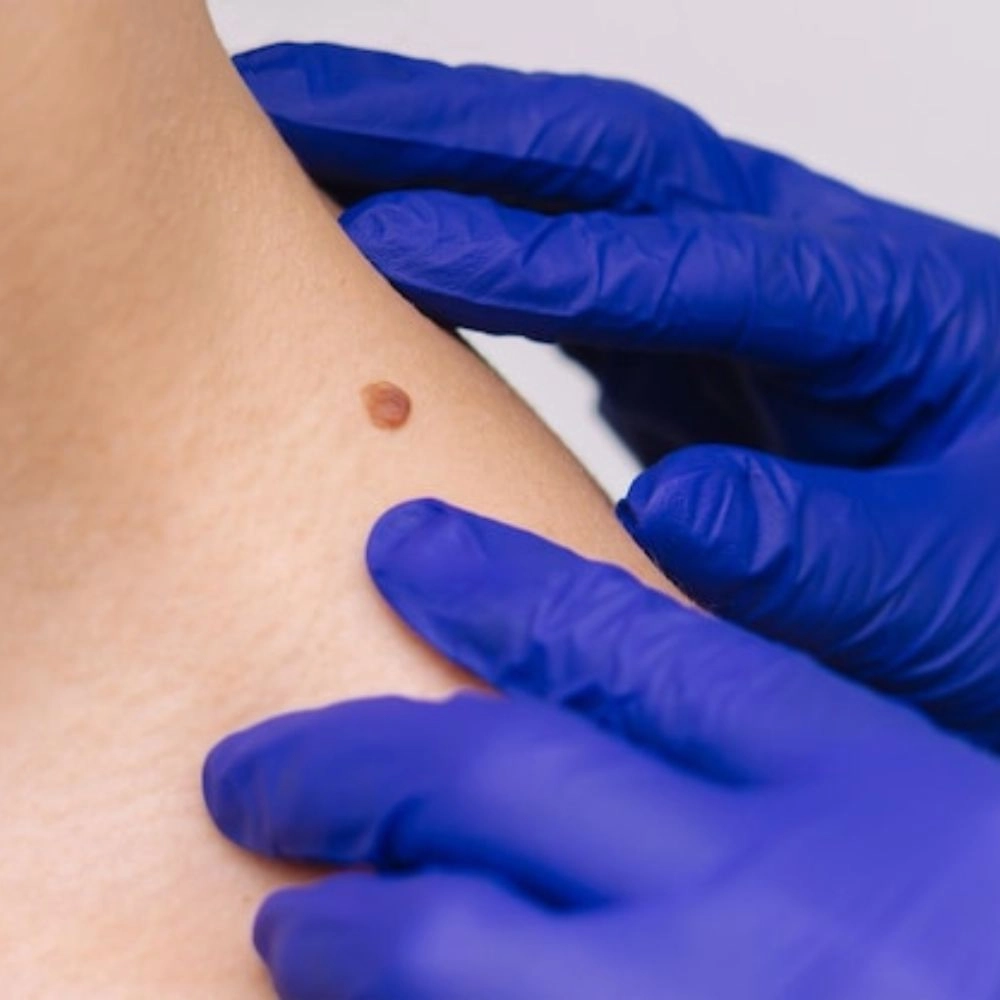
INDICATION – DEFINITION
A nevus, more commonly known as a mole, is a growth on the skin due to a proliferation of melanocytes, which are the cells that produce the pigment in your skin. There are several types of nevi, including congenital nevi, dysplastic nevi, and acquired nevi, each with their unique features and implications.
Clinical Causal Factors
- Genetics: Nevus development is often hereditary. Certain genetic mutations or conditions can increase the likelihood of nevi. For example, people with familial atypical multiple mole-melanoma (FAMMM) syndrome are at an increased risk of developing atypical (dysplastic) nevi and melanoma.
- Immune Status: Patients with a compromised immune system, such as those with HIV/AIDS or organ transplant recipients taking immunosuppressive medications, may have an increased risk of developing nevi.
- Hormonal Changes: Hormonal changes during puberty, pregnancy, or when taking contraceptives can lead to the development or change in nevi.
Non-Clinical Causal Factors
- Sun Exposure: Ultraviolet (UV) radiation from the sun or tanning beds can stimulate the growth of moles. A history of sunburns or intense sun exposure, especially during childhood, can increase the risk of developing nevi and potentially skin cancer.
- Age: The number of moles usually peaks in young adulthood and decreases with age, though some may persist.
- Skin Type: Individuals with lighter skin, hair, and eyes, are more prone to having moles, as are people who sunburn easily.
While most moles are benign, they can sometimes turn into melanoma, a serious type of skin cancer. Regular skin examinations are crucial for early detection of any changes in the shape, color, size, or symptoms (such as itching or bleeding) of a mole, which could potentially be signs of malignancy.
SYMPTOMS AND DIAGNOSIS
Symptoms
- Color: Nevi can be pink, tan, brown, black, or a mix of these. They may darken with sun exposure and during pregnancy.
- Shape/Size: Most are oval or round. They may be flat or raised and typically less than 6 millimeters in diameter, though they can be larger.
- Location: Nevi can appear anywhere on the skin.
- Change: While nevi can naturally change over time, sudden changes in size, color, or shape, or new symptoms like itching, pain, bleeding, or ulceration should be evaluated by a dermatologist.
Diagnosis
A dermatologist will first perform a visual inspection, possibly with a dermatoscope, a tool that provides magnified, illuminated view of the skin. If a mole looks suspicious, a biopsy may be performed. In a biopsy, a small piece of skin is removed and examined under a microscope to check for cancer cells.
The ‘ABCDE rule’ can help identify atypical moles that may have turned cancerous:
- Asymmetry: One half of the mole doesn’t match the other.
- Border: The edges are irregular or blurred.
- Color: There are various shades in one mole.
- Diameter: The mole is larger than 6mm.
- Evolving: The mole is changing in size, shape or color.
Always consult a dermatologist if you notice any unusual changes in your moles.
Prognosis and Impact

Most nevi are benign and do not cause any significant medical problems. They are common and often harmless, even if you have many. However, a change in the size, shape, or color of a mole, or the development of new symptoms, such as itching or bleeding, can be a sign of melanoma, a serious form of skin cancer. Early detection and treatment of melanoma are critical for a favorable prognosis.
Even benign moles can have a psychological impact on individuals, particularly if they are large, numerous, or located on visible areas of the body. This can affect self-esteem and quality of life.
When a mole becomes malignant, it can be life-threatening. Melanoma can spread to other parts of the body, which complicates treatment and worsens the prognosis. The 5-year survival rate for localized melanoma (has not spread) is 99%, but for metastatic melanoma (has spread), it drops to about 27%.
Therefore, regular self-examination and dermatologist visits are crucial for early detection of any suspicious changes in your moles. Prevention, especially sun protection, is also key.
Treatment Options
Watchful Waiting: For most benign moles, no treatment is necessary, but regular monitoring for changes in size, color, shape, or new symptoms is essential.
Surgical Removal: If a mole is suspicious for malignancy, it can be completely removed (excisional biopsy) or partially removed (incisional biopsy) for further examination under a microscope. If confirmed to be a melanoma, further surgery might be required to remove any remaining cancer and possibly nearby lymph nodes.
Laser Removal: Some benign moles can be removed with laser treatment, though this method isn’t typically used for moles that are deeply embedded in the skin or have any signs of being malignant, because the laser only treats the top layers of skin and does not allow for pathological examination.
Topical Treatments: In some cases, particularly for certain types of pre-cancerous lesions, a doctor might recommend a topical cream, such as imiquimod or fluorouracil, to help stimulate the body’s immune system to fight off abnormal cells.
For malignant moles, additional treatments like radiation therapy, chemotherapy, immunotherapy, or targeted therapy may be needed, depending on the stage and spread of the cancer.
Risks and Side Effects
Watchful Waiting: There is a small risk that a mole being monitored might change and become malignant. Regular self-examination and routine skin checks by your dermatologist can help detect these changes early.
Surgical Removal: Risks associated with mole removal surgery include infection, bleeding, allergic reaction to anesthesia, and nerve damage. There can be a scar after the mole has been removed, and there’s a small chance that the mole can recur after removal.
Laser Removal: Risks with laser mole removal include infection, scarring, and changes in skin color. Also, if the mole is malignant, the laser might not be able to remove cancer cells deep within the skin, allowing them to potentially grow and spread.
Topical Treatments: Topical treatments like imiquimod or fluorouracil can cause redness, irritation, blistering, or discoloration of the skin. There can be a local allergic reaction, and rarely, systemic side effects if absorbed in significant amounts.
For malignant moles, additional treatments like radiation therapy, chemotherapy, immunotherapy, or targeted therapy may be needed. These treatments can cause a wide range of side effects, such as fatigue, nausea, hair loss, skin problems, weakened immune system, etc.
FAQ Section
A nevus, commonly known as a mole, is a growth on the skin that develops when pigment-producing cells (melanocytes) grow in clusters. Most people have moles, and they are generally harmless.
The formation of a nevus is primarily influenced by genetics and sun exposure. Certain hormonal changes, like during puberty or pregnancy, can also lead to the development or changes in moles.
Most nevi are benign or non-cancerous. However, in some cases, they can turn into melanoma, a serious type of skin cancer. Regular self-examination and routine skin checks by a dermatologist are important for early detection.
Signs of a possibly malignant mole include changes in size, color, or shape, asymmetry, irregular borders, diameter greater than 6mm, and any new symptoms like itching, pain, or bleeding.
A dermatologist will examine the suspicious mole visually and may use a tool called a dermatoscope. If the mole appears atypical, a biopsy may be performed, which involves removing a small piece of skin to be examined under a microscope.
Treatment options depend on the mole’s nature. Most benign moles require no treatment, but regular monitoring is recommended. Suspicious moles may be surgically or laser removed. If a mole is found to be malignant, treatments can include surgery, chemotherapy, radiation therapy, immunotherapy, or targeted therapy.
Potential side effects and risks depend on the treatment type and can range from minimal (such as minor scarring after removal) to more significant (like side effects associated with chemotherapy or immunotherapy). It’s crucial to discuss these with your healthcare provider.
Sun protection is key. Avoiding intense sun exposure, especially during peak UV times, and regularly using a broad-spectrum sunscreen can help prevent nevus formation and reduce the risk of skin cancer.
It’s recommended to perform self-examinations of your skin once a month and to have a professional skin examination by a dermatologist annually, or more often if you’re at a higher risk.
