Last Updated: August 22, 2023
Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
Moderate Burn Scar
INDICATION – BRIEF
Moderate burn scars are typically a result of second-degree burns that damage both the outer and deeper skin layers. Clinical factors affecting scarring include the depth, extent, and location of the burn, infection, and healing time. Non-clinical factors include age, nutrition, genetic predisposition, smoking habits, and sun exposure. Children, the elderly, and smokers often experience more severe scarring, as do individuals with poor nutrition or a genetic predisposition to scarring. Therapies for moderate burn scars can include silicone treatments, pressure garments, corticosteroid injections, or surgery, depending on the scar’s size, location, and functional or aesthetic impact.
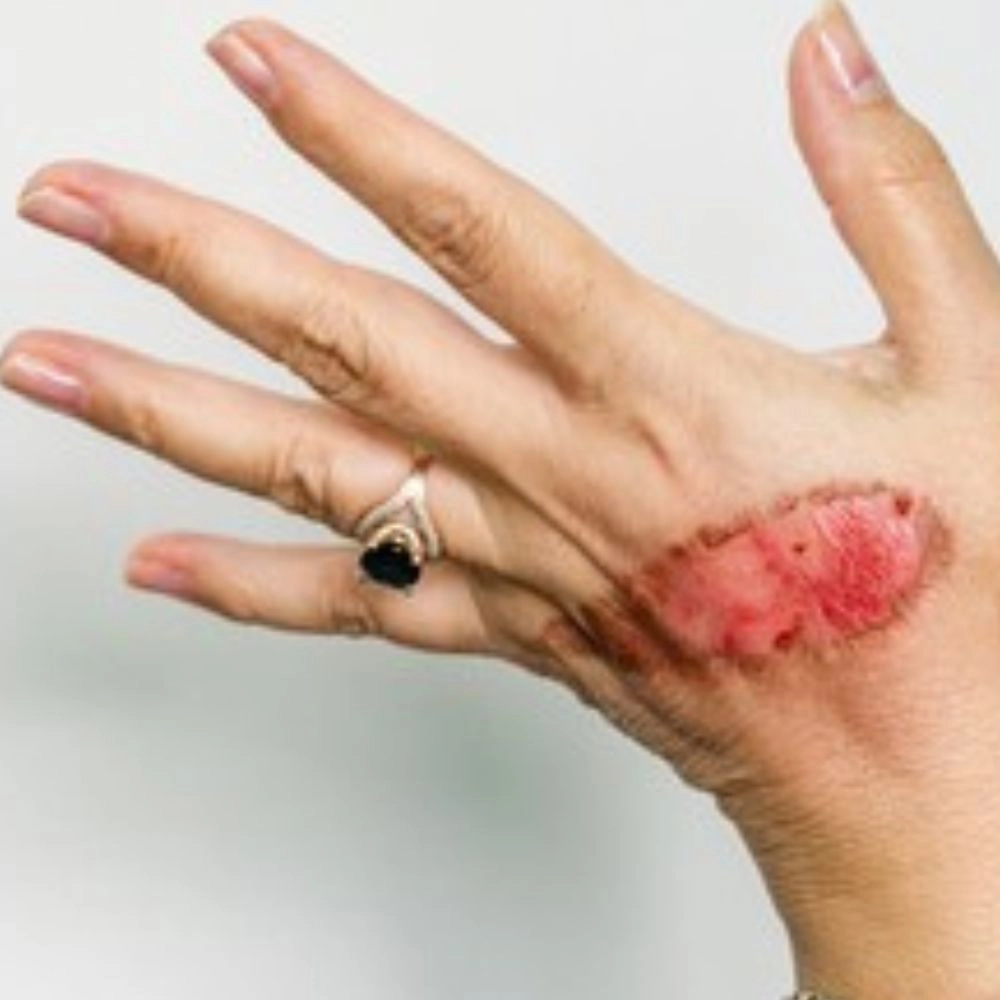
INDICATION – DEFINITION
Moderate burn scars are typically a result of second-degree burns. These burns injure the epidermis (the outer layer of skin) and part of the dermis (the deeper layer of skin). These types of burns often heal with scarring, which varies depending on the severity and extent of the injury.
Clinical Causal Factors
Clinical factors that can influence the formation and extent of moderate burn scars include:
- Depth and extent of burn: The more severe and widespread the burn, the more likely it is to cause a significant scar.
- Location of burn: Certain areas of the body, such as the face, hands, feet, and major joints, are more prone to severe scarring.
- Infection: Infections can exacerbate the damage caused by a burn and can lead to more significant scarring.
- Healing time: The longer a burn wound takes to heal, the more likely it is to scar. In general, burns that take more than 2-3 weeks to heal will often result in scarring.
Non-Clinical Causal Factors
Non-clinical factors can also influence the development and severity of scarring. These include:
- Age: Children and elderly people may scar more severely than young adults, due to the differences in their skin’s elasticity and healing capacity.
- Nutrition: Good nutrition, particularly adequate protein intake, is essential for proper wound healing and can reduce the likelihood of severe scarring.
- Genetic factors: Some people are genetically predisposed to form more severe scars, including hypertrophic scars and keloids.
- Smoking: Smoking can impair wound healing and increase the risk of scarring.
- Sun exposure: Exposure to sun can darken the scar and make it more noticeable.
Management of moderate burn scars may involve various therapies such as silicone sheets or gels, pressure garments, corticosteroid injections, or surgical revision in certain cases. Each case is unique, and the management strategy will depend on factors such as the scar’s location, size, and impact on function or appearance.
SYMPTOMS AND DIAGNOSIS
Symptoms
- Color changes: The scarred area may appear redder, darker, or lighter than the surrounding skin.
- Texture changes: The scar may be raised (hypertrophic) or indented (atrophic), and the skin may be tougher or smoother than the surrounding skin.
- Sensitivity changes: The area may be more sensitive to touch, temperature, or sun exposure, or it might be less sensitive due to damaged nerve endings.
- Restricted movement: If the scar is located near a joint or is large, it can limit the range of motion.
- Pain or discomfort: Depending on the depth and location of the scar, it may cause ongoing pain or discomfort.
- Itching: Many burn scars can be itchy, especially during the healing process.
Diagnosis
Diagnosis of a moderate burn scar is primarily based on a physical examination of the skin. The doctor will evaluate the burn’s size, depth, and location and any associated symptoms like pain, itchiness, or restricted movement. They may also inquire about the burn incident, including the cause and any treatments administered.
In some cases, further diagnostic testing may be necessary, particularly if there’s concern about deep tissue damage or if the scar is not healing as expected. This can include imaging tests like an ultrasound, CT scan, or MRI, or a skin biopsy where a small sample of the scar tissue is removed and examined under a microscope.
Ultimately, the goal of diagnosing a burn scar is not only to assess the scar itself but also to guide the most effective treatment approach. Treatment options are determined based on the scar’s characteristics and the patient’s overall health and personal preferences.
Prognosis and Impact

Prognosis
The outlook for a moderate burn scar varies greatly and is influenced by factors like the size and depth of the original burn, the body’s healing capacity, and the treatment received. While some scars may become less noticeable over time, most burn scars are permanent. The color, texture, and other characteristics of the scar can often be improved with treatment, but typically, the scar cannot be completely removed.
It’s also important to note that new symptoms can develop over time. For example, a scar might initially seem soft and flat, but it can become raised and hard (hypertrophic) or even form a keloid (an overgrowth of scar tissue) over time.
Impact
Moderate burn scars can have significant physical and psychological impacts.
- Physical Impact: Physically, a scar can cause discomfort, itchiness, pain, and sensitivity to temperature or touch. If the scar is near a joint, it can restrict movement and cause functional impairment.
- Psychological Impact: The psychological impact can be substantial, particularly if the scar is in a highly visible location. It can lead to self-consciousness, decreased self-esteem, anxiety, or depression. The experience of the burn injury itself can also contribute to psychological distress or post-traumatic stress disorder (PTSD).
- Social Impact: There can be social implications as well, as people with visible scars often report feeling stigmatized or experiencing social isolation.
Management of burn scars therefore involves a holistic approach, addressing not just the physical appearance of the scar, but also the functional and psychological effects. It can include medical treatments, physical therapy, and psychological support, such as counseling or support groups. The goal is to help the individual regain as much function and comfort as possible and to assist in their psychological adjustment to the scar.
Treatment Options
- Topical Treatments: Silicone sheets or gels are commonly used as they can flatten and soften scars and reduce associated symptoms like redness and itching. Other topical treatments include creams or gels with ingredients like onion extract or vitamin E, although their efficacy can vary.
- Pressure Therapy: Pressure garments may be recommended for larger or more severe scars. These are custom-made, tight-fitting clothes that apply pressure to the scarred area, helping to reduce scar height and thickness.
- Corticosteroid Injections: These can help to flatten and soften hypertrophic scars or keloids.
- Laser Therapy: Various types of lasers can be used to improve the color, texture, and thickness of scars. Some lasers can also help to relieve symptoms like itchiness or pain.
- Surgical Revision: In some cases, surgery may be considered to improve the scar’s appearance or to increase the range of motion if the scar is restricting movement. This can involve excising the scar and re-closing the wound, or other techniques like skin grafting or tissue expansion.
- Physical Therapy: If the scar is near a joint or restricts movement, physical therapy can help to improve flexibility and function.
- Psychological Support: Due to the significant psychological impact of burn scars, counseling or support groups may be beneficial to help the individual cope with any feelings of self-consciousness, anxiety, or depression related to the scar.
Risks and Side Effects
- Topical Treatments: Silicone sheets or gels are generally well-tolerated, but some people may experience skin irritation or an allergic reaction. Similarly, creams or gels may cause irritation, redness, or a rash in some individuals.
- Pressure Therapy: Pressure garments can be uncomfortable and hot to wear and may cause skin irritation. They need to be worn consistently for many months, and compliance can sometimes be an issue, particularly in children.
- Corticosteroid Injections: Side effects can include pain at the injection site, skin thinning, or changes in skin color. Rarely, these injections can cause systemic effects, such as elevated blood sugar levels or hormonal imbalances.
- Laser Therapy: Potential risks and side effects depend on the specific type of laser used but can include pain, redness, swelling, and temporary changes in skin color. More serious complications, such as burns or scarring, are rare but possible.
- Surgical Revision: As with any surgery, there’s a risk of bleeding, infection, and anesthetic complications. There’s also the possibility that the scar revision may not improve the appearance of the scar as much as hoped, or it could potentially worsen the scar’s appearance.
- Physical Therapy: There may be temporary discomfort or pain associated with exercises and movements during physical therapy sessions.
- Psychological Support: In general, psychological support has few risks, but opening up about personal experiences and feelings can sometimes be emotionally challenging.
FAQ Section
A moderate burn scar typically results from a second-degree burn that damages both the outer and deeper skin layers. It often leaves a scar which may be darker, lighter, or redder than the surrounding skin and may be raised or indented.
Factors such as the depth and extent of the burn, its location, the presence of infection, the healing time, age, nutrition, genetic factors, smoking habits, and sun exposure can all influence the severity of a moderate burn scar.
A moderate burn scar is diagnosed primarily based on a physical examination of the skin. In some cases, further diagnostic testing such as imaging tests or a skin biopsy may be necessary.
Physically, a scar can cause discomfort, itchiness, pain, and may restrict movement. Psychologically, the scar can lead to self-consciousness, decreased self-esteem, anxiety, or depression. It’s also possible to experience social challenges due to stigma or isolation.
Treatments can range from topical applications like silicone sheets or gels, pressure therapy, corticosteroid injections, laser therapy, surgical revision, physical therapy, to psychological support.
While treatments for moderate burn scars are generally safe, they can carry certain risks or side effects, such as skin irritation, discomfort, changes in skin color, or even rare serious complications. It’s important to discuss these risks with your healthcare provider.
While treatments can significantly improve the appearance and symptoms of a moderate burn scar, most burn scars are permanent and complete removal is unlikely. The goal of treatment is to reduce the scar’s visibility, improve functionality and comfort, and provide psychological support.
While not all burns can be prevented, immediate and appropriate treatment of a burn injury can reduce the likelihood of severe scarring. This includes cooling the burn, keeping the area clean, using appropriate dressings, and seeking medical attention.
