Last Updated: August 22, 2023
Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
Mild Burn Scar
INDICATION – BRIEF
Mild burn scars are often the result of first or superficial second-degree burns, primarily affecting the epidermis or part of the dermis layer. Clinical causes include the initial burns and improper wound care, or infections. Non-clinical factors involve genetic predisposition to scarring, aging, poor nutrition, and environmental factors like sun exposure and dry air. Treatment for mild burn scars varies depending on factors such as the scar’s size and location, the patient’s age and overall health, and the patient’s perception of the scar, ranging from conservative measures like creams and massage to more invasive procedures like surgery or laser therapy. Always consult with a healthcare provider for proper diagnosis and treatment.
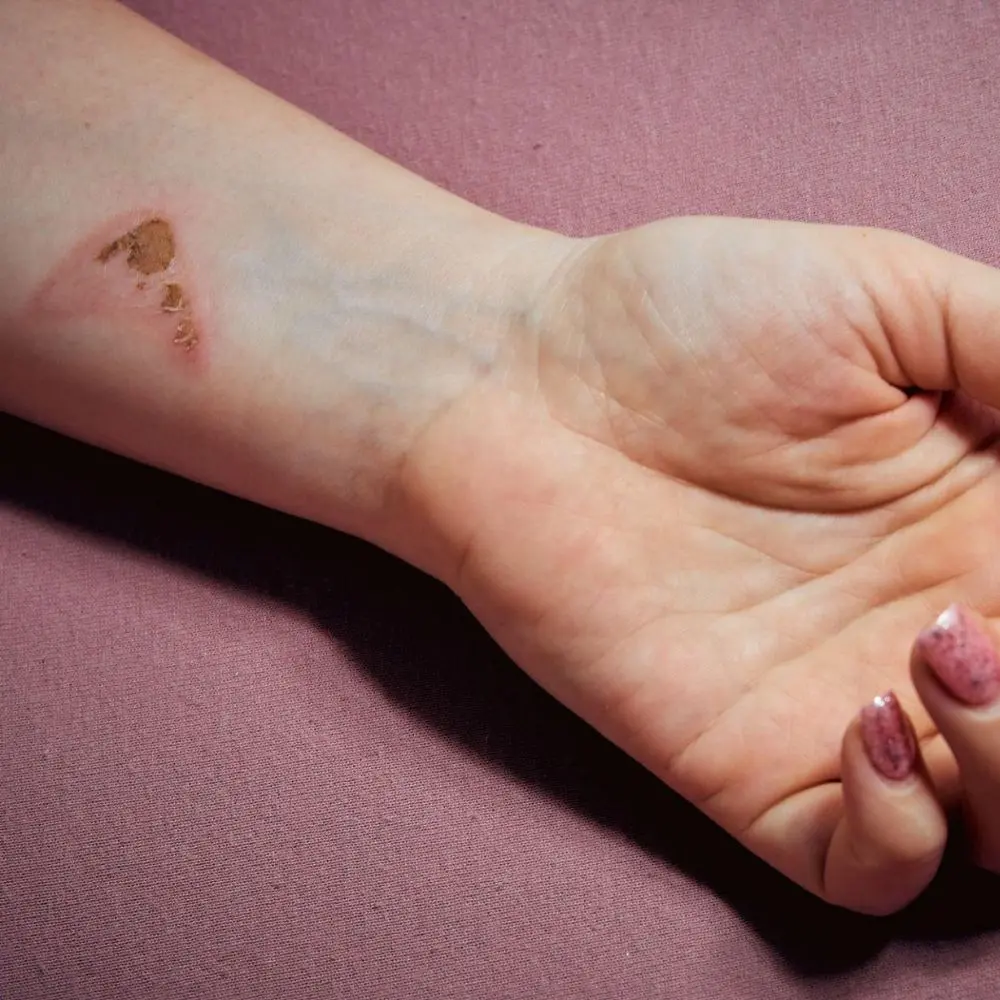
INDICATION – DEFINITION
Mild burn scars are typically the result of first or superficial second-degree burns that affect the outermost layer of skin, the epidermis, and potentially part of the dermis layer. These burns can leave a scar, but the severity is usually lower compared to deeper burns.
Clinical Factors
- Clinical Causes:
- Burns: The most direct cause is burns from various sources like heat, radiation, electricity, chemicals, and even certain types of friction.
- Inappropriate Wound Care: Inappropriate or inadequate care of the initial burn can result in scarring. This could include delayed treatment, improper cleaning, and dressing of the wound, or not following prescribed care.
- Infection: If the burn wound becomes infected, it can delay healing and increase the likelihood of a scar.
Non-Clinical Factors
- Genetic Factors: Some people have a genetic predisposition to form scars more easily than others.
- Age: Older skin tends to be less resilient and may scar more easily following a burn.
- Nutrition: Good nutrition is essential for proper wound healing. Lack of certain nutrients, like vitamin C and protein, can hinder the healing process and increase the likelihood of scarring.
- Environmental Factors: Exposure to sunlight can cause scars to darken. Moreover, dry air can make the skin less elastic, and prone to scarring.
The indications for treating mild burn scars can vary widely based on factors like the location and size of the scar, the age and health of the patient, and the patient’s personal feelings about the scar. Treatment options can range from conservative methods such as silicone sheets, gels, creams, and massage, to more invasive procedures like laser therapy, surgery, or injections.
SYMPTOMS AND DIAGNOSIS
Symptoms
Mild burn scars can present with several symptoms including:
- Visual Change: The skin might look discolored, typically redder, lighter, or darker than the surrounding skin. The skin texture might be different as well, being either smoother or rougher.
- Sensitivity: The scarred area can be more sensitive to the touch or temperature changes.
- Itching: The area may itch, especially during the healing process and the early stages of scar formation.
- Pain or Discomfort: Even mild scars can sometimes cause discomfort or a mild ache.
- Tightness: Scars can feel tight, particularly when they are over a joint or large area.
Diagnosis
Mild burn scars are typically diagnosed based on a combination of the patient’s history and a physical examination.
- Patient’s History: The doctor will ask about the original injury, the care it received, and any symptoms you’re currently experiencing.
- Physical Examination: The doctor will visually inspect the scar and may touch it to assess its texture, elasticity, and any changes in the skin color or quality.
In some cases, the doctor might refer the patient to a specialist like a dermatologist or a plastic surgeon for further assessment and treatment suggestions. The specialist might use devices like a dermatoscope, which magnifies the skin area for a detailed view, or order additional tests like a biopsy if there are concerns about the scar.
Prognosis and Impact

Prognosis
The prognosis for mild burn scars is generally quite good, particularly with appropriate care and management. These types of scars often become less noticeable over time, usually over months to years, and can sometimes almost completely disappear.
The healing process and the final appearance of the scar can be influenced by several factors such as the individual’s age, overall health, nutrition, genetics, as well as the quality of the initial wound care and follow-up care. With proper wound care, infection prevention, and scar management techniques such as massage, silicone sheets or gels, and sun protection, scar appearance can be significantly minimized.
Impact
The impact of a mild burn scar can vary greatly depending on its location, size, and the individual’s personal feelings about it.
- Physical Impact: Mild burn scars can cause physical discomfort, including itching, tenderness, or sensitivity to temperature changes. If located over a joint, they might also limit mobility due to skin tightness.
- Psychological Impact: Even mild scars can have a psychological impact. They can affect self-esteem and body image, potentially leading to feelings of embarrassment or self-consciousness, especially if they’re in a visible location.
- Social Impact: These feelings can extend to social situations, influencing how an individual interacts with others or participates in social activities.
It’s essential for healthcare providers to address all these factors when caring for someone with a burn scar. This can include referring the person to a mental health professional if the psychological or social impacts are significant.
Treatment Options
- Topical Treatments:
- Silicone Sheets and Gels: Silicone has been shown to be effective in reducing scar size, improving skin hydration, and mitigating scar color.
- Creams and Oils: Moisturizing creams and oils can help hydrate the skin and may improve elasticity, reducing the risk of the scar feeling tight or itchy.
- Physical Therapy:
- Massage: Regularly massaging the scar can improve its flexibility and reduce any feelings of tightness or itchiness.
- Medical Procedures:
- Steroid Injections: These can help to reduce inflammation and can make the scar flatter and softer.
- Laser Therapy: Certain types of lasers can improve the appearance, texture, and color of scars.
- Surgery: In some cases, surgery may be recommended to revise the scar. This is typically considered for scars that limit mobility, are painful, or are aesthetically unacceptable to the patient.
- Psychosocial Interventions: Due to the potential psychological impact of scarring, interventions like cognitive-behavioral therapy (CBT) can be used to help patients cope with their scars, if needed.
Each treatment option has its own benefits, risks, and contraindications. Therefore, the decision on which treatment to use should be individualized based on the patient’s condition, scar characteristics, and preferences.
Risks and Side Effects
- Topical Treatments:
- Silicone Sheets and Gels: Some people may have an allergic reaction to silicone. Irritation, redness, or discomfort in the area of application may also occur.
- Creams and Oils: The risks are generally low but can include skin irritation, allergic reactions, or worsening of the scar if the product is not suitable or used improperly.
- Physical Therapy:
- Massage: Massage should be gentle and not cause pain. If performed too vigorously, it can cause discomfort, skin irritation, or potentially even harm the healing tissue.
- Medical Procedures:
- Steroid Injections: Risks include pain at the injection site, skin color changes, and the possibility of making the scar worse by causing a depression in the skin if the steroid is injected too deeply.
- Laser Therapy: Potential side effects include pain during treatment, temporary redness, swelling, changes in skin color, blistering, and rarely, scarring.
- Surgery: Surgical risks include infection, bleeding, and anesthetic complications. There’s also a risk that the surgery might not improve the scar’s appearance or that a new scar may form.
- Psychosocial Interventions:
- Cognitive-behavioral therapy (CBT): While CBT is generally considered low-risk, some people may experience distress or emotional discomfort when discussing or confronting issues related to their scar.
FAQ Section
Mild burn scars are typically the result of first or superficial second-degree burns. Factors that can impact scar development include the type of burn, the quality of initial wound care, infection, genetics, nutrition, and environmental factors like sun exposure.
Mild burn scars may cause changes in skin color and texture, increased sensitivity, itching, mild pain, and a feeling of tightness. The scarred area may look different from the surrounding skin and feel different to the touch.
A healthcare provider typically diagnoses mild burn scars based on the patient’s history and a physical examination. In certain cases, they might refer you to a specialist for a more detailed evaluation.
The prognosis is generally good. Mild burn scars often become less noticeable over time and may almost completely disappear. Factors such as age, overall health, genetics, and quality of wound care can influence the healing process and final appearance of the scar.
Treatments can range from topical treatments like silicone sheets and gels to medical procedures such as steroid injections, laser therapy, or surgery. Physical therapies like massage can also be beneficial. In some cases, psychological interventions may be helpful to address the emotional impact of scarring.
Yes, each treatment comes with potential risks or side effects, including allergic reactions, skin irritation, pain, temporary redness, swelling, changes in skin color, and, in rare cases, scarring from certain treatments. Discuss these in detail with your healthcare provider to understand what to expect.
While it’s not always possible to prevent scarring completely, early and proper wound care can help minimize scar formation. This includes cleaning the wound, applying antibiotic cream, and keeping the wound covered. Consult with your healthcare provider for appropriate care instructions.
