Last Updated: August 22, 2023
Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
KELOID SCARS
INDICATION – BRIEF
Keloid scars are raised, irregular scars that form due to an overzealous healing process, extending beyond the original injury. Clinically, genetic predisposition, skin type, age, gender, and injury location play a role. People with darker skin tones and those under 30 are more susceptible. Non-clinically, physical trauma, inflammatory conditions, and prolonged skin tension contribute. While any skin injury can lead to a keloid, areas under tension or with inflammation are more prone. Treatment ranges from corticosteroid injections and laser therapy to surgery, but recurrence is high. Prevention is ideal and can involve avoiding procedures like piercings or tattoos in prone individuals.
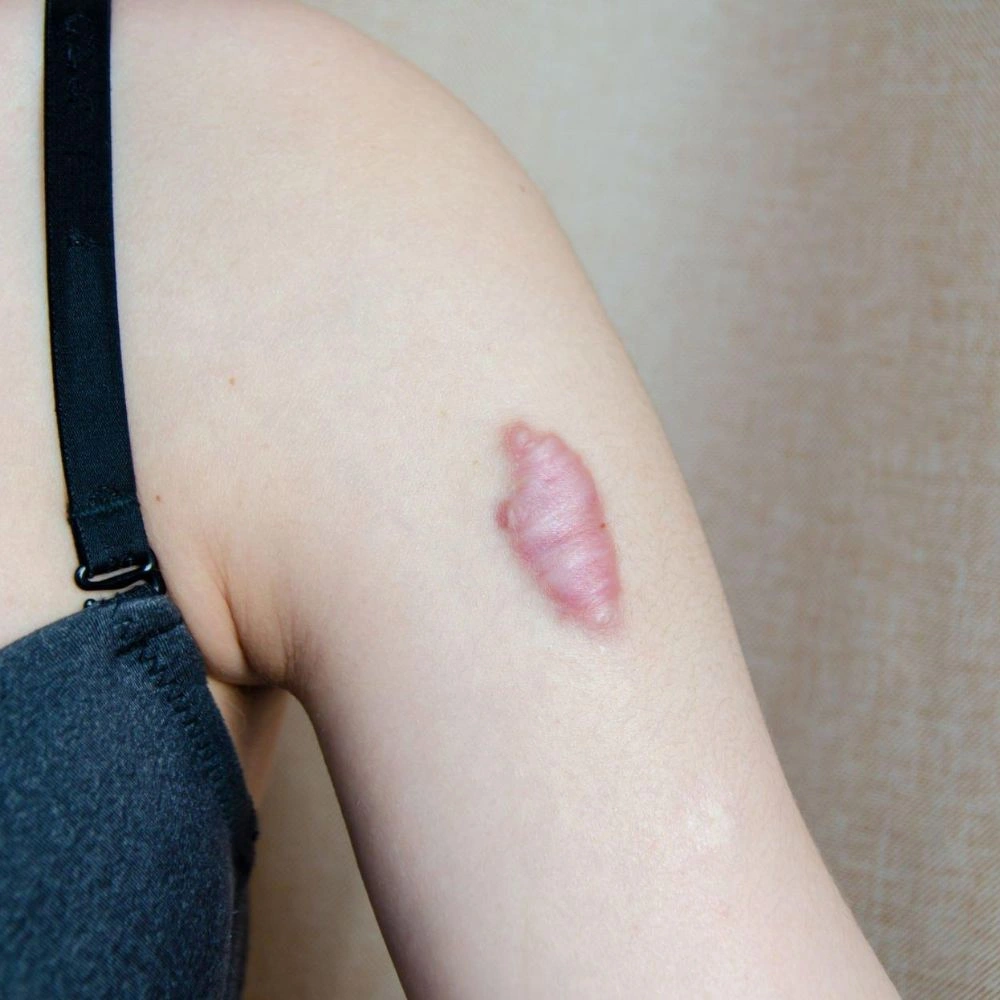
INDICATION – DEFINITION
Keloid scars are a type of scar that develops due to an overly aggressive healing process. They extend beyond the original injury site, forming a raised, often shiny, irregularly shaped scar. These scars can occur following surgical incisions, traumatic wounds, vaccination sites, burns, acne, or even minor injuries such as ear piercings.
Clinical Causal Factors
- Genetic Predisposition: Keloids tend to occur more often in people with a family history of keloids. Certain genetic changes may make some individuals more susceptible to developing these types of scars.
- Skin Type: People with darker skin tones, such as African, Hispanic, and Asian descent, are more prone to developing keloids.
- Age and Gender: Keloids can occur at any age, but they’re more common in people under the age of 30. Both men and women are equally likely to have keloids, though some studies suggest they might be slightly more common in women, possibly related to instances such as piercings or certain types of surgery.
- Location of Injury: Keloids are more common in areas of the body where the skin is naturally tight, such as the chest, back, shoulders, and earlobes.
Non-Clinical Causal Factors
- Physical Trauma: Any skin injury can lead to a keloid. This includes cuts, burns, acne scars, chickenpox scars, ear piercing, tattooing, or surgical incision sites.
- Inflammatory Conditions: Conditions that cause inflammation in the skin, such as acne or infections, may also lead to keloid scarring.
- Prolonged Skin Tension: Areas of the body where the skin is kept under tension for prolonged periods, such as the shoulders or chest, may be more prone to developing keloids.
Treatment for keloids includes intralesional corticosteroid injections, laser therapy, cryotherapy, radiation therapy, or surgical removal. However, it should be noted that keloids have a high rate of recurrence even after treatment. The approach is typically to minimize the symptoms and appearance, rather than completely eradicate the scar, as the triggering of the healing process can lead to the formation of a new keloid. Use of pressure garments or silicone sheets can also help to reduce the size of keloids over time.
Prevention, where possible, is preferable. This may include avoiding elective procedures such as piercings or tattoos in individuals with a known predisposition to keloid formation. If surgery is necessary, steps can be taken post-operatively, like using silicone sheets or injections, to reduce the likelihood of keloid formation.
SYMPTOMS AND DIAGNOSIS
Symptoms
Symptoms of Keloid Scars:
Keloid scars manifest as raised, thickened areas of skin that are usually pink, red, or flesh-colored. They can form on any part of the body but are most common on the chest, back, shoulders, and earlobes. Key symptoms include:
- Growth Beyond Injury Site: Unlike typical scars, keloids expand beyond the boundary of the original wound.
- Texture and Appearance: Keloids have a shiny, hard, and rubbery texture.
- Persistent Growth: Keloids continue to grow slowly over time.
- Discomfort or Pain: Keloids can cause discomfort, itching, or even pain, particularly when they are in the growth phase.
- Interference with Movement: If a keloid develops over a joint or skin crease, it may restrict movement.
Diagnosis
Diagnosis of Keloid Scars:
The diagnosis of keloids is typically made based on clinical examination and patient history. The characteristics of the scar, its location, and history of how it has evolved are generally enough to differentiate it from other types of scars.
- Physical Examination: Dermatologists can typically diagnose a keloid based on its appearance. The key characteristic is the growth of the scar beyond the original wound border.
- Medical History: A detailed medical history is important to understand any prior incidents of keloid formation, history of trauma or injury, and any family history of keloid formation.
- Biopsy: In some cases, if the diagnosis is not clear-cut, a skin biopsy might be performed where a small piece of the scar is removed and examined under a microscope to confirm the diagnosis.
Prognosis and Impact

Prognosis
Keloid scars are benign, noncancerous growths and do not pose a direct threat to one’s life. However, their management can be challenging due to the high recurrence rate after removal. It is important to note that while treatments can improve the appearance of keloids and alleviate symptoms like pain or itchiness, they rarely eliminate the scar completely.
- Recurrence: Even after undergoing treatment, keloids often return, and in some cases, they may grow back larger than before. This is because the treatment procedures themselves can cause skin injury, which triggers the keloid formation process. Recurrence rates after surgical removal alone can be as high as 45-100%.
- Long-Term Management: Considering the high recurrence rate, managing keloids often requires a long-term strategy, usually a combination of treatments such as surgery, followed by steroid injections, laser therapy, or radiation therapy, and regular follow-ups.
Impact
Impact of Keloid Scars:
The impact of keloid scars goes beyond the physical symptoms. They can have significant psychological and social implications.
- Cosmetic Concerns: Given their appearance, keloids can lead to self-consciousness, embarrassment, or distress, especially if they are in visible areas like the face or neck.
- Psychological Impact: People with keloids may experience anxiety, depression, and a decreased quality of life due to the appearance of the scars and associated symptoms.
- Physical Discomfort: Large or poorly located keloids can interfere with movement, especially if they’re located near a joint. They can also cause discomfort, itchiness, or even pain.
- Social Isolation: Some individuals may withdraw from social activities due to self-consciousness about their appearance, leading to feelings of isolation.
Managing keloids, therefore, often requires a holistic approach that not only addresses the physical symptoms but also offers support for any psychological distress caused by the condition.
Treatment Options
Keloid scars can be particularly challenging to treat due to their high recurrence rate. The most effective treatment approach is often a combination of different methods. Here are some of the commonly employed treatment options:
- Intralesional Corticosteroid Injections: These are often the first-line treatment for keloids. Steroids reduce inflammation and slow down the rapid cell proliferation that characterizes keloids. Injections are typically given every 4 to 6 weeks until the scar flattens out.
- Cryotherapy: This involves freezing the keloid from the surface of the skin using liquid nitrogen. It can help reduce the hardness and size of the keloid, but multiple treatments are often necessary.
- Laser Therapy: Different types of lasers can be used to reduce the redness and improve the texture of keloids. Lasers can also be used to remove the keloid altogether, often in combination with other treatments.
- Surgical Removal: This is usually reserved for larger keloids or those that haven’t responded to other treatments. However, surgery can sometimes trigger the formation of a similar or even larger keloid.
- Radiation Therapy: This is usually used in conjunction with surgical removal. Radiation is applied immediately after surgery to reduce the risk of the keloid returning.
- Silicone Sheets or Gels: They are applied directly to the keloid, often for several months, to help flatten and soften the scar.
- Pressure Therapy: It involves using bandages or specially designed pressure devices to apply constant pressure to the keloid, which can help reduce its size.
Each of these treatments has its advantages and disadvantages, and their effectiveness can vary from person to person.
Risks and Side Effects
- Intralesional Corticosteroid Injections: These can cause pain at the injection site, skin discoloration, and atrophy (thinning of the skin). Some people may also experience systemic side effects such as weight gain, fluid retention, and high blood pressure, especially with repeated injections.
- Cryotherapy: This can cause pain during the procedure and temporary skin discoloration. The scar may also become larger or more raised following treatment.
- Laser Therapy: Possible side effects include pain during the procedure, temporary redness or swelling, skin discoloration, and a slight risk of scarring or infection.
- Surgical Removal: The major risk is the recurrence of an even larger keloid. Other potential risks include those common to all surgeries, such as infection, bleeding, and adverse reactions to anesthesia.
- Radiation Therapy: While effective, radiation therapy comes with a very slight increased risk of cancer, particularly in younger patients. Other side effects include temporary redness, blistering, or darkening of the skin.
- Silicone Sheets or Gels: These are generally well-tolerated, but some people may experience skin irritation, rashes, or discomfort.
- Pressure Therapy: It can be uncomfortable and requires consistent use for many hours a day, which some people may find inconvenient. There may also be skin irritation or breakdown under the pressure device.
FAQ Section
Keloid scars are caused by an overactive healing response after the skin has been damaged. They can develop from surgical wounds, cuts, burns, acne, chickenpox scars, and even minor skin damage like ear piercings. Certain people, particularly those with darker skin tones and a family history of keloids, are more prone to developing them.
Unlike regular scars that remain within the boundary of the original injury, keloids extend beyond this area and form a raised, thickened patch of skin. They continue to grow and don’t naturally diminish over time as other scars typically do.
While treatments can significantly improve the appearance of keloids and alleviate symptoms like itching or discomfort, they often don’t completely eliminate the scar. Keloids have a high recurrence rate after treatment. A combination of treatments usually provides the best outcome.
No, keloid scars are benign, noncancerous growths. However, they can lead to discomfort, aesthetic concerns, and potential psychological distress.
If you’re prone to keloids, you might want to avoid unnecessary skin damage such as tattoos, piercings, or elective surgeries. If surgery is unavoidable, your healthcare provider can take steps to minimize the risk of keloids, such as using minimal-tension wound closure techniques, applying silicone sheets, or giving steroid injections post-operatively.
No, not all skin injuries lead to keloids. It’s a combination of the individual’s genetic predisposition, skin type, and the type, location, and severity of skin damage.
Several treatment options are available, including corticosteroid injections, cryotherapy, laser therapy, surgery, radiation therapy, silicone sheets or gels, and pressure therapy. A combination of these treatments often provides the best results. It’s important to consult with a healthcare professional to decide the best treatment plan for you.
