Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
FUNGAL NAILS
INDICATION – BRIEF
Fungal nails, or onychomycosis, is an infection that discolors, thickens, and can cause the nail to crumble. Clinical factors contributing to this condition include aging, poor circulation, immunosuppression, skin injury, and pre-existing skin conditions. Non-clinical factors include moist environments, certain occupations, lifestyle habits like wearing non-breathable footwear, poor personal hygiene, and sharing personal items. Fungi thrive in warm, moist places and can spread via shared items. Diagnosis typically involves laboratory tests and treatment may include antifungal medications or, in severe cases, nail removal. Preventive measures like good hygiene and avoiding shared grooming tools are key due to the stubborn nature of this condition.
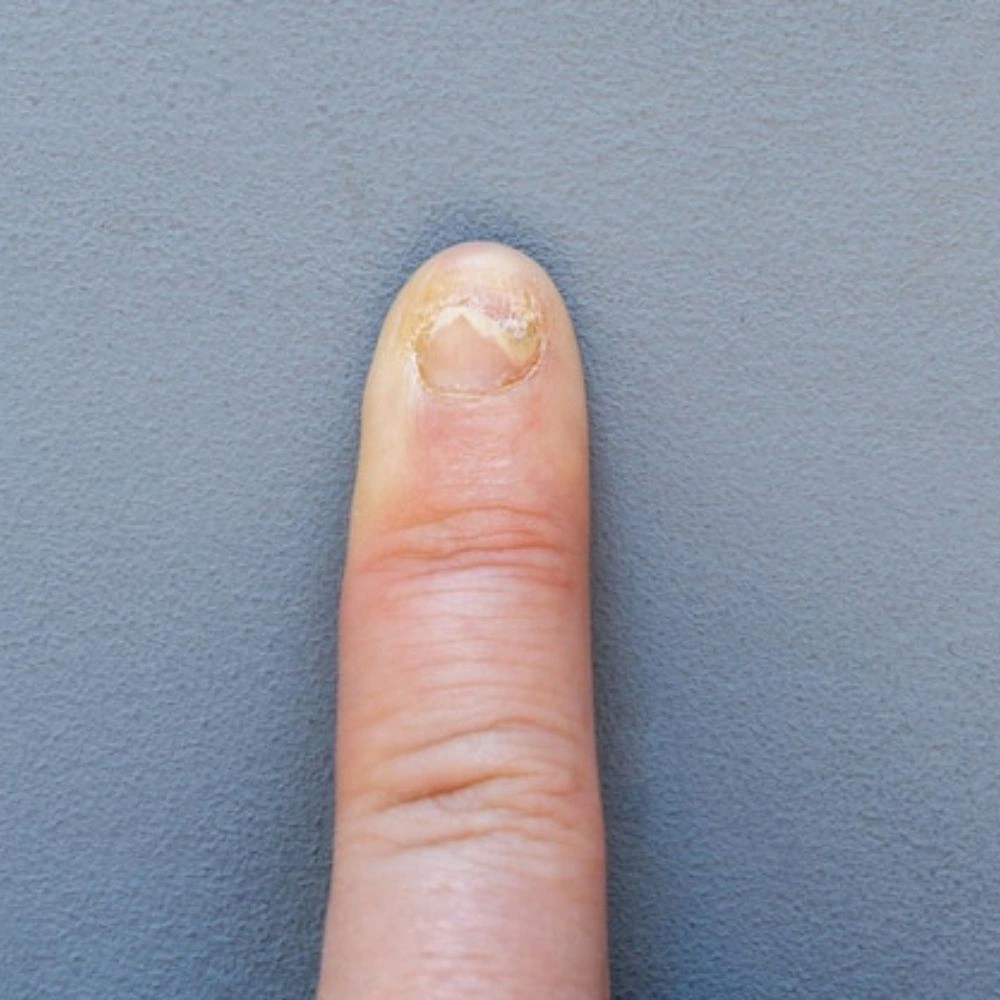
INDICATION – DEFINITION
Let’s look into the causes and factors that may predispose an individual to this condition:
Clinical Factors
- Aging: Older adults are more prone to nail fungus due to a slower growing nail and increased years of exposure to fungi.
- Poor Circulation: Conditions that affect blood circulation, like peripheral artery disease or diabetes, increase the risk of developing nail fungus.
- Immunosuppression: A weakened immune system due to conditions like HIV/AIDS or certain medications can lead to a higher risk of fungal infections.
- Skin Injury: Any minor injury near the nail, like a cut or an ingrown nail, can provide an entry point for the fungus.
- Pre-existing skin conditions: Certain skin conditions, such as psoriasis or dermatitis, can also increase the susceptibility to nail fungus.
Non-clinical factors
- Environment: Fungi are microscopic organisms that don’t need sunlight to survive. They often thrive in warm, moist environments, like showers, swimming pools, and locker rooms.
- Occupational Hazard: Jobs that require hands to be wet for long periods, like bartending or housekeeping, can lead to fungal nail infections.
- Lifestyle Habits: Wearing socks and shoes that hinder ventilation and do not absorb perspiration can provide an ideal environment for fungi to thrive.
- Personal Hygiene: Not maintaining proper hygiene and cleanliness can predispose to fungal infections.
- Sharing items: Sharing items such as nail clippers, shoes, or socks with a person who has a nail fungus can also increase the risk of getting a fungal nail infection.
The diagnosis of fungal nails is typically confirmed through laboratory tests, including KOH tests, fungal cultures, or nail biopsies. Antifungal medications, both oral and topical, are commonly used treatments. In some severe cases, the affected nail may need to be removed.
It’s important to note that nail fungus can be stubborn, and recurrences are common. Therefore, prevention plays a key role in managing this condition. Maintaining good hygiene, wearing breathable footwear, and avoiding shared grooming tools can help to prevent nail fungus.
SYMPTOMS AND DIAGNOSIS
Symptoms
- Discoloration: The nail may become white, yellow, brown or green.
- Thickening: As the fungal infection progresses, the nail often becomes thicker and harder to cut.
- Distorted Shape: The nail may become warped or distorted in shape.
- Brittleness: The nail might crumble or split, often at the edges initially.
- Debris under the nail: As the fungus spreads, you might notice buildup of debris under the nail.
- Smell: In some cases, a slightly foul odor may be present.
- Pain: While not always present, some people might experience pain or discomfort, particularly in severe infections or if the nail separates from the nail bed.
Diagnosis
The diagnosis of fungal nail infections is typically confirmed through a clinical examination and specific laboratory tests.
- Clinical Examination: Your dermatologist would initially examine the nail visually. They may also take your medical history to understand potential risk factors.
- Laboratory Tests: If a fungal infection is suspected, a sample of your nail or the debris under your nail will be taken and sent to a lab.
- KOH test: This is a quick test where the sample is mixed with potassium hydroxide, which dissolves the nail material and leaves behind the fungi, if present.
- Fungal culture: This test involves growing the fungi from your sample in a lab. This helps in identifying the exact type of fungus causing the infection.
- Histology: In some cases, a nail biopsy may be needed. This test uses a special stain that makes the fungus more visible under a microscope.
These steps ensure an accurate diagnosis, helping your dermatologist to determine the best course of treatment for you. It’s important to get an accurate diagnosis as other conditions, like psoriasis, can mimic the symptoms of a fungal nail infection.
Prognosis and Impact

Impact
The impact of fungal nails varies between individuals and often depends on the severity of the infection and the person’s overall health.
- Physical Discomfort: While some people might experience physical discomfort or pain, especially in severe cases or if the nail separates from the nail bed, most cases of onychomycosis are not painful.
- Cosmetic Concern: One of the most significant impacts of fungal nails is the cosmetic concern. The discoloration, thickening, and crumbling of the nail can cause embarrassment or distress, leading to reduced self-esteem and quality of life, especially for those who have jobs or lifestyles where their hands or feet are frequently visible.
- Impact on Daily Activities: In severe cases, the thickening of the nails may cause discomfort when walking or wearing shoes, thus affecting daily activities.
- Secondary Infections: If left untreated, fungal nail infections can potentially lead to secondary bacterial infections, particularly in individuals with a weakened immune system. This can lead to cellulitis, a more serious skin infection.
- Spread of Infection: Onychomycosis can spread to other nails, and in some cases, to other people if they come into direct contact with infected nails or use shared items like nail clippers, socks, or shoes.
It’s important to seek medical attention for suspected fungal nails to minimize these impacts. Treatment options include topical and oral antifungal medications, laser treatment, or, in more severe cases, surgical nail removal. By combining appropriate treatment with preventive measures like good foot hygiene, wearing breathable shoes and socks, and avoiding shared personal grooming tools, you can improve your prognosis and lessen the impact of this condition.
Treatment Options
- Topical treatments: These include antifungal creams, ointments, and nail lacquers such as ciclopirox. These are generally more effective in mild cases, particularly when the infection is caught early. Topical treatments need to be applied daily for several months.
- Oral antifungal drugs: These are often the first line of treatment for more severe fungal nail infections. Medications such as terbinafine and itraconazole help a new nail grow free of infection, slowly replacing the infected part of your nail. You typically take these medications for 6 to 12 weeks, but you won’t see the end result of treatment until the nail grows back completely.
- Medicated nail polish: Your doctor may prescribe an antifungal nail polish called ciclopirox (Penlac). You paint it on your infected nails and surrounding skin once a day. After seven days, you wipe the piled-on layers clean with alcohol and begin fresh applications.
- Medicated nail cream: Your doctor may prescribe an antifungal cream, which you rub into your infected nails after soaking. These creams may work better if you first thin the nails. This helps the medication get through the hard nail surface to the underlying fungus.
- Laser and light-based therapies: More recent developments in the treatment of onychomycosis include the use of laser or other light-based therapies. These treatments heat and kill the fungi, but more research is needed to test long-term success rates of these methods.
- Surgery: In severe cases or if the infection is causing significant pain, the nail can be removed surgically. However, a new nail will usually grow back, though it might take a year or so. If the area of infected nail is small, you may be able to avoid having the entire nail removed by having just the infected section done.
Risks and Side Effects
- Topical treatments: While these are typically well-tolerated, they can sometimes cause skin irritation, redness, swelling, burning, or itching at the application site. The main risk is that they may not be as effective in severe cases, as it’s hard for them to penetrate the nail plate to reach the underlying fungus.
- Oral antifungal drugs: These are generally effective but may cause side effects such as rash, upset stomach, liver damage, and changes in taste. Your doctor will monitor your liver function during treatment. Those with liver disease or heart failure should inform their doctor before starting these medications.
- Medicated nail polish: Potential side effects include redness and irritation of the skin around the nail. It can also lead to an abnormal nail shape or color if used for a long time.
- Medicated nail cream: Similar to other topical treatments, the cream can cause skin irritation at the application site. Also, its effectiveness may be limited as it has to penetrate the nail to reach the fungus.
- Laser and light-based therapies: These are generally safe procedures with minimal side effects. However, there may be a sensation of heat or minor pain during the procedure. Post-procedure, temporary nail discoloration and minor nail bed injury can occur.
- Surgery: Risks associated with nail removal include pain, infection, swelling, and delay or lack of nail regrowth. There is also a risk that the infection may return after the nail regrows.
FAQ Section
Onychomycosis, also known as fungal nails, is a common condition that begins as a white or yellow spot under the tip of your fingernail or toenail. As the fungal infection goes deeper, it may cause your nail to discolor, thicken, and crumble at the edge.
Fungal nail infections are caused by various fungal organisms (fungi). The most common cause is a type of fungus called dermatophyte. Aging, poor circulation, a weakened immune system, skin injuries, and exposure to fungus-infested environments are factors that can increase the risk of getting a fungal nail infection.
Symptoms may include discoloration, thickening, shape distortion, brittleness, debris under the nail, a slightly foul odor, and occasionally pain in the affected nail.
Diagnosis is typically confirmed through a clinical examination and specific laboratory tests, such as a KOH test, fungal culture, or, in some cases, a nail biopsy. These help to identify the presence and type of fungus causing the infection.
Treatment options include topical and oral anti-fungal medications, medicated nail polish or cream, laser and light-based therapies, and in severe cases, surgery to remove the infected nail.
Yes, each treatment option can have side effects. Topical treatments can cause skin irritation, while oral antifungal drugs can cause upset stomach, liver damage, and changes in taste. Medicated nail polish or cream can lead to skin irritation and abnormal nail shape or color. Laser and light-based therapies may cause temporary nail discoloration and minor nail bed injury, while surgery carries risks such as pain, infection, and delay in nail regrowth.
Yes, preventive measures include maintaining good foot hygiene, wearing breathable shoes and socks, avoiding shared personal grooming tools, and minimizing exposure to fungus-infested environments.
