Table of content
- Types of BREAST RECONSTRUCTION
- Procedure
- Risks and complications
- Pre-operation preparation
- Post-operative care
- Expected Results and recovery timeline
- Appointments and consultation
- Frequently asked questions
- Meet the team
- Pricing and payment plans
- Medical literature and research
- Support and counseling
- Send a message
ANDROGENIC ALOPECIA
INDICATION – BRIEF
Androgenic alopecia is a genetically influenced type of hair loss. Clinical factors include genetics, hormonal changes, aging, and certain medical conditions like PCOS. Non-clinical factors encompass stress, nutritional deficiencies, and lifestyle habits like smoking. The condition typically manifests as gradual thinning at the hairline, increasing hair loss at the top of the head in men, and overall thinning in women. Diagnosis generally relies on hair loss patterns and family history, sometimes supplemented with a scalp biopsy. Treatments range from medications like minoxidil or finasteride to hair transplants, scalp reduction surgery, or low-level laser therapy.
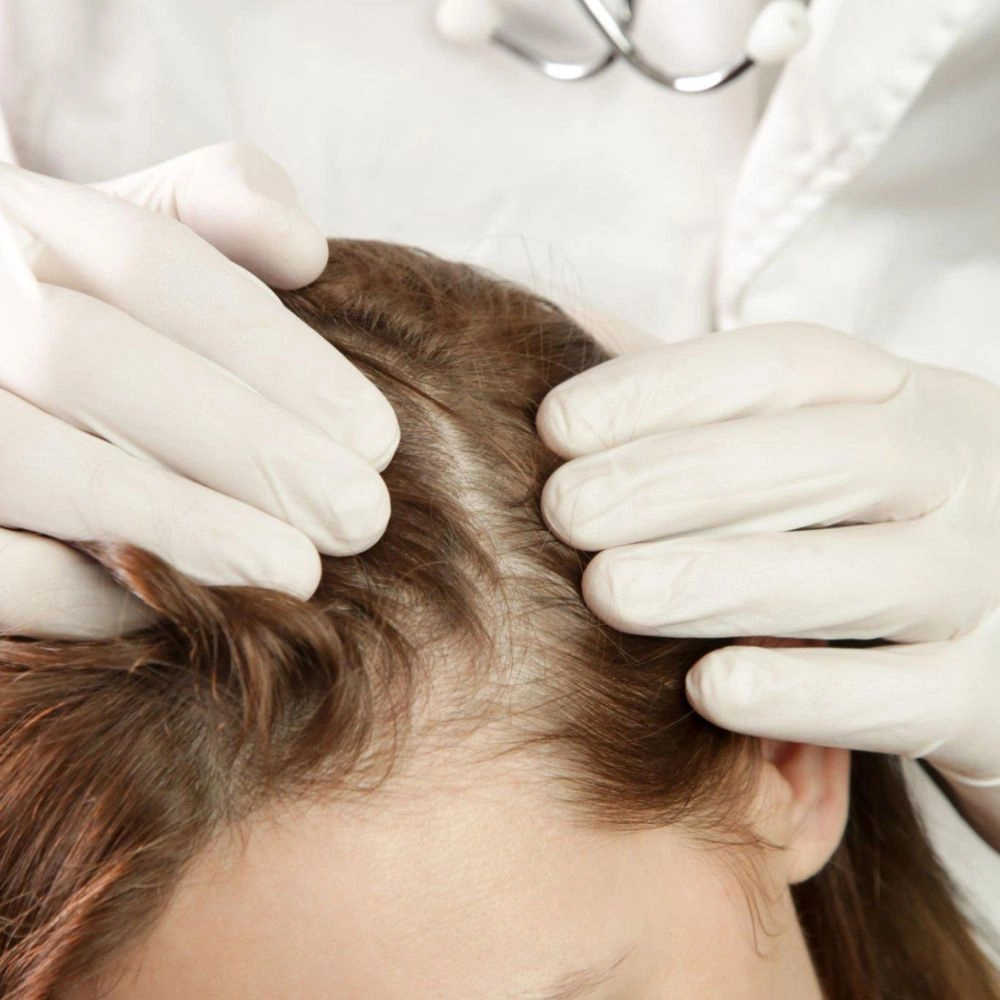
INDICATION – DEFINITION
Androgenic alopecia, also known as male-pattern baldness or female-pattern hair loss, is a type of hair loss that is genetically determined and influenced by androgens, which are hormones like testosterone.
Clinical factors that can contribute to androgenic alopecia include
- Genetics: This is the most significant risk factor. If your parents or grandparents have hair loss, you may also develop it.
- Hormonal changes: Androgens play a crucial role in the development of male-pattern baldness. An enzyme called 5-alpha reductase converts testosterone to dihydrotestosterone (DHT) in hair follicles, which can lead to hair follicle miniaturization and a shorter hair growth cycle.
- Age: The prevalence and rate of hair loss increase with age.
- Medical conditions: Conditions like polycystic ovary syndrome (PCOS), which is associated with elevated androgen levels, can cause androgenic alopecia in women.
Non-clinical factors may also contribute to the condition
- Stress: High-stress levels may exacerbate genetic hair loss by increasing the body’s production of adrenaline, which can be converted into cholesterol and then into DHT in the hair follicles.
- Nutrition: Severe nutritional deficiencies, including iron, vitamin D, and certain B vitamins, can contribute to or exacerbate hair loss.
- Lifestyle: Smoking has been associated with androgenic alopecia, possibly because it damages the DNA of the hair follicle.
Androgenic alopecia typically starts with gradual thinning at the hairline, followed by increasing hair loss at the top of the head. In women, hair generally thins all over the head, but the frontal hairline is usually preserved.
Diagnosis is typically based on the pattern of hair loss and family history. A scalp biopsy may be necessary in some cases to rule out other causes of hair loss.
Treatment can include medication like minoxidil (Rogaine) or finasteride (Propecia, Proscar), as well as certain procedures like hair transplants or scalp reduction surgery. Low-level laser therapy is also a possible treatment. Remember, every treatment has its benefits and risks, so discussing these options with a dermatologist is important.
SYMPTOMS AND DIAGNOSIS
Symptoms
In androgenic alopecia, the pattern of hair loss differs between men and women. In men, it often starts with a receding hairline and then proceeds to thinning or balding on the top (crown) of the head. The hair at the back of the head is typically less affected. In women, androgenic alopecia usually involves general thinning of the hair, especially at the crown, but the frontal hairline is often preserved.
Another symptom might be a change in the hair’s quality before it starts falling out. Hair may become thinner or shorter, and the time it spends in the growing phase may reduce. This is called miniaturization of the hair follicles.
Diagnosis
Diagnosis of androgenic alopecia is usually based on the pattern and history of hair loss, along with a family history of similar hair loss. A dermatologist will perform a physical examination, observing the pattern of hair loss, the condition of the hair and scalp, and any signs of other concurrent diseases that might be contributing to the hair loss.
In some cases, additional tests may be conducted:
- Pull Test: A dermatologist might pull out about 60 hairs and look at them under a microscope to determine the phase of growth and whether they are being shed prematurely.
- Scalp Biopsy: If the cause of hair loss is still unclear, a small piece of the scalp might be removed and examined under a microscope. This can help identify or rule out the possibility of infection or other conditions.
- Blood Tests: If other symptoms suggest hormonal imbalances, autoimmune diseases, or other health issues, blood tests might be conducted.
Please note that treatment and management should be personalized for each individual based on the cause and severity of the hair loss, as well as the individual’s preference and overall health.
Prognosis and Impact

Prognosis
Androgenic alopecia is a progressive condition, meaning it tends to worsen over time. While the speed and pattern of progression can vary greatly from person to person, those who begin losing hair at a younger age often experience more extensive baldness. In some men, the hairline will continue to recede until all or most of the hair is gone.
For women, the hair loss is usually more evenly spread out across the top of the scalp and does not tend to result in total baldness. The progression of hair loss in women is often slower than in men.
Despite the progressive nature of androgenic alopecia, it’s important to note that this condition doesn’t affect physical health. There’s no medical necessity to treat it unless it’s causing significant psychological distress.
Impact
The impact of androgenic alopecia is mainly psychological and can be significant. In a society that often equates hair with youth, attractiveness, and health, experiencing hair loss can lead to a decrease in self-esteem and can cause anxiety or depression in some individuals.
It’s important to note that these feelings are completely normal, and there are resources available to help individuals cope. These resources include mental health professionals and support groups for individuals dealing with hair loss.
For those who wish to treat their hair loss, there are options available, including medical treatments and surgical procedures. However, the effectiveness of these treatments varies from person to person, and they can carry potential side effects. It’s always best to have a thorough discussion with your dermatologist about the pros and cons of these treatment options.
Treatment Options
- Topical Agents: Minoxidil (Rogaine) is an over-the-counter medication applied directly to the scalp. It prolongs the growth phase of hair follicles and can slow hair loss in some people.
- Oral Medications: Finasteride (Propecia) is a prescription medication for men that reduces levels of DHT, a key contributor to hair loss. It’s taken orally and can slow hair loss and even lead to regrowth in some men. Dutasteride (Avodart) is a similar medicine that might be used if finasteride is not effective.
- Hair Transplant Surgery: This involves removing small plugs of hair from areas where hair is still growing and placing them in areas that are balding. This can be quite effective but can also be expensive and cause scarring.
- Scalp Reduction Surgery: This is a more drastic surgical option where sections of the scalp with hair are pulled forward to fill in a bald spot.
- Low-Level Laser Therapy (LLLT): This uses light to stimulate hair growth. Although research is still ongoing, some studies suggest it could help with hair loss.
- PRP Therapy: Platelet-Rich Plasma (PRP) Therapy involves injecting the patient’s own platelets into the scalp to promote hair growth. Some studies have shown promising results, but more research is needed.
- Lifestyle Changes: Improving diet, reducing stress, and abstaining from smoking can potentially slow hair loss.
It’s important to remember that not all treatments will work for all patients, and these options can have side effects. Consultation with a healthcare provider is essential to determine the best course of action for any individual. Additionally, since androgenic alopecia is progressive, treatment might need to be continued long-term to maintain its effects.
Risks and Side Effects
- Topical Agents (Minoxidil): Possible side effects can include scalp irritation, dryness, scaling, itching, and/or redness. In rare cases, it can cause unwanted hair growth on the face and hands. An allergic reaction is also possible.
- Oral Medications (Finasteride, Dutasteride): These can potentially cause decreased sex drive, erectile dysfunction, ejaculation disorders, and enlarged breasts in men. Pregnant women should avoid contact with these medications as they could harm a male fetus.
- Hair Transplant Surgery: Risks include infection, scarring, unnatural-looking tufts of new hair growth, and the transplanted hair might not grow as well as expected. There’s also the potential risk associated with any surgical procedure, such as bleeding or adverse reactions to anesthesia.
- Scalp Reduction Surgery: This surgery carries risks such as infection, scarring, and the potential for an unnatural look. Other surgical risks include bleeding and adverse reactions to anesthesia.
- Low-Level Laser Therapy (LLLT): This therapy is generally well-tolerated, but some patients may experience scalp irritation, redness, or discomfort.
- PRP Therapy: As this uses the patient’s own blood, the risk of an allergic reaction is low. However, any injection can cause infection, injury, or nerve damage. There may also be some pain and scalp tenderness after the procedure.
- Lifestyle Changes: Generally, lifestyle changes pose minimal risks but depending on the change (like altering diet), they might have unintended consequences. It’s advisable to consult a healthcare provider when making significant lifestyle changes.
All treatments should be discussed thoroughly with a healthcare provider, who can explain their potential benefits and risks. It’s also worth noting that these treatments may need to be used long-term to maintain their effects, and their effectiveness varies from person to person.
FAQ Section
Androgenic alopecia is primarily caused by genetic and hormonal factors. Increased sensitivity to androgens (male hormones) in hair follicles can lead to hair loss. Other factors like age, stress, certain medical conditions, and nutritional deficiencies can also contribute.
Yes, while it’s more common in men, women can also experience androgenic alopecia, usually presenting as overall thinning of hair.
Diagnosis is usually based on the pattern of hair loss, family history, and a medical evaluation. Additional tests like scalp biopsy or blood tests may be done if needed.
Currently, there’s no cure for androgenic alopecia, but there are treatments available that can slow the progression and sometimes stimulate regrowth. The effectiveness varies among individuals.
Treatment options include topical agents like minoxidil, oral medications like finasteride, hair transplant surgery, scalp reduction surgery, low-level laser therapy, and PRP therapy.
Yes, all treatments can potentially have side effects. These can range from scalp irritation with minoxidil to sexual side effects with finasteride, or risks associated with surgery like infection and scarring.
In most cases of androgenic alopecia, hair loss is permanent. Treatments can potentially stimulate hair regrowth, but it’s usually necessary to continue the treatment to maintain the benefits.
Yes, lifestyle changes like managing stress, maintaining a balanced diet, and quitting smoking can potentially slow hair loss.
While androgenic alopecia itself isn’t a sign of a serious medical condition, it can sometimes be associated with other medical conditions like polycystic ovary syndrome (PCOS) in women.
Yes, hair shedding (telogen effluvium) is often temporary and can be caused by various factors like stress or illness. Androgenic alopecia, on the other hand, is a long-term condition that leads to permanent hair loss in a specific pattern.
